-
 Written By
Prabakar Mahalingam
Written By
Prabakar Mahalingam
- Published
What Is a Defibrillator? A Complete Guide to How Defibrillators Work

Reviewed by Prabakar Mahalingam, Managing Partner at AED Total Solution. Prabakar is a nationally recognized provider of safety training, products, and proprietary compliance software dedicated to addressing Sudden Cardiac Arrest (SCA).
A defibrillator is a medical device that delivers a controlled electrical shock to restore a normal heart rhythm during sudden cardiac arrest (SCA). The most widely used type in public settings is the Automated External Defibrillator (AED), a portable, battery-operated device that anyone can use without medical training.
Each year, more than 356,000 people experience out-of-hospital cardiac arrest in the United States, according to the American Heart Association. Approximately 10,000 of those events occur in the workplace. When a bystander uses an AED within the first three to five minutes, survival rates can increase from less than 10% to nearly 70%, making defibrillators the most effective intervention for SCA outside of a hospital.
This comprehensive guide covers everything you need to know about defibrillators: how they work, the four main types, when they are used, AED requirements for workplaces, and how to choose the right defibrillator for your organization.
Quick Answer: What Is a Defibrillator?
A defibrillator is a device that delivers an electrical shock to the heart to treat life-threatening cardiac arrhythmias, specifically ventricular fibrillation (VF) and pulseless ventricular tachycardia (pVT). In public settings, AEDs are the most common type. They analyze the heart rhythm automatically, determine whether a shock is needed, and guide the user through the process with voice prompts. No medical license or certification is required to operate an AED.
How Does a Defibrillator Work?
A defibrillator works by delivering a precise electrical current through the heart muscle. This current momentarily depolarizes all the heart’s muscle cells at once, stopping the chaotic electrical activity that prevents the heart from pumping blood. After this reset, the heart’s natural pacemaker (the sinoatrial node) has the opportunity to re-establish a coordinated, life-sustaining rhythm.
Here is the step-by-step process that occurs during defibrillation:
- Electrode pad placement. Two adhesive electrode pads are placed on the patient’s bare chest, typically in the anterolateral position: one on the upper right chest below the collarbone and one on the lower left side below the armpit. For detailed placement instructions, see our AED pad placement guide.
- Heart rhythm analysis. The device analyzes the patient’s heart rhythm through the electrode pads. Modern defibrillators use advanced algorithms to identify two specific shockable heart rhythms: ventricular fibrillation (VF) and pulseless ventricular tachycardia (pVT).
- Energy delivery. If a shockable rhythm is detected, the device charges its internal capacitor and delivers a controlled electrical shock. Most modern devices use biphasic waveform technology, which the AHA has recognized as more effective and requiring lower energy levels than older monophasic systems.
- Post-shock reassessment. After the shock, the device re-analyzes the heart rhythm. If a normal rhythm has not been restored, the device may prompt for another shock. CPR should continue between analysis cycles to maintain blood flow to the brain and vital organs.
The entire defibrillation process takes only seconds. Research published in the Journal of the American College of Cardiology has shown that each minute of delay in defibrillation reduces the probability of survival by 7% to 10%. This is why early access to a defibrillator is critical.
The Four Types of Defibrillators
Defibrillators are categorized into four main types, each designed for different clinical settings and user types. Understanding the differences is essential for organizations deciding how to protect their employees, students, or visitors.
1. Automated External Defibrillator (AED)
An AED is a lightweight, portable device designed specifically for use by non-medical personnel. It is the type of defibrillator found in workplaces, schools, airports, gyms, houses of worship, and other public locations.
Key features of AEDs:
- Automatically analyzes heart rhythm and determines if a shock is needed
- Guides the user through each step with voice prompts and visual indicators
- Built-in safeguards prevent a shock from being delivered unless a shockable rhythm is detected
- Available in semi-automatic (user presses a button to deliver the shock) and fully automatic (shock is delivered without user intervention) models
- Battery-operated and requires minimal maintenance (periodic battery and pad replacement checks)
- All AEDs sold in the U.S. must be FDA-approved
AEDs are the most relevant type of defibrillator for organizational preparedness. If you are evaluating AEDs for your workplace, our comparison of the best portable AED defibrillators provides detailed reviews of top models from Philips, ZOLL, Defibtech, and Cardiac Science. For information on AED pricing and total cost of ownership, see our complete buyer’s guide.
2. Manual External Defibrillator
Manual defibrillators are used by paramedics, emergency physicians, and other trained medical professionals in hospitals and ambulances. Unlike AEDs, they require the operator to interpret the heart rhythm on a monitor and manually select the energy level and timing of each shock.
These devices offer more control and are capable of both defibrillation (for VF/pVT) and synchronized cardioversion (for other arrhythmias like atrial fibrillation). Manual defibrillators are not appropriate for public access or untrained users.
3. Implantable Cardioverter-Defibrillator (ICD)
An ICD is a small device surgically implanted inside the body, typically below the collarbone. It continuously monitors the patient’s heart rhythm and automatically delivers an internal shock if it detects a life-threatening arrhythmia.
ICDs are prescribed for patients who have survived cardiac arrest or who are at high risk for dangerous heart rhythms due to conditions like heart failure, hypertrophic cardiomyopathy, or genetic arrhythmia syndromes. For a detailed comparison of ICDs and other implanted cardiac devices, see our guide on ICD vs. pacemaker differences.
4. Wearable Cardioverter-Defibrillator (WCD)
A WCD is a vest-like garment worn outside the body that continuously monitors the heart and can deliver a shock if needed. It is typically prescribed as a temporary measure for patients who are at risk for SCA but are not yet candidates for an ICD, for example, after a heart attack or while waiting for cardiac surgery.
The most widely known WCD is the LifeVest by ZOLL Medical. Unlike an ICD, a WCD does not require surgical implantation and can be removed at any time.
Defibrillator Comparison Table
| Feature | AED | Manual | ICD | WCD |
|---|---|---|---|---|
| Who uses it | General public | Medical professionals | Patient (automatic) | Patient (automatic) |
| Training required | None (recommended) | Advanced medical | None (implanted) | Basic orientation |
| Location | External, portable | External, hospital/EMS | Internal, surgically implanted | External, wearable vest |
| Rhythm analysis | Automatic | Manual by operator | Automatic | Automatic |
| Typical cost | $1,200–$3,000+ | $10,000–$35,000 | $30,000–$50,000 (with surgery) | $3,000–$4,000/month |
| Best for | Workplaces, schools, public spaces | Hospitals, ambulances | High-risk cardiac patients | Temporary cardiac risk |
When Is a Defibrillator Used?
A defibrillator is used during sudden cardiac arrest, which occurs when the heart suddenly stops beating effectively due to an electrical malfunction. SCA is different from a heart attack (which is a circulation problem caused by a blocked artery). For a detailed comparison, see our article on sudden cardiac arrest vs. heart attack.
The two heart rhythms that a defibrillator can treat are:
- Ventricular fibrillation (VF): The heart’s lower chambers quiver chaotically instead of contracting, producing no blood flow. VF is the most common initial rhythm in witnessed cardiac arrest. Learn more in our ventricular fibrillation guide.
- Pulseless ventricular tachycardia (pVT): The heart beats dangerously fast but produces no detectable pulse, meaning no effective blood circulation.
A defibrillator will not deliver a shock for non-shockable rhythms such as asystole (flatline) or pulseless electrical activity (PEA). If the AED analyzes the rhythm and determines no shock is needed, it will instruct the user to continue CPR. For more about what happens in this scenario, see AED says no shock advised.
Signs That Someone Needs a Defibrillator
Recognizing sudden cardiac arrest quickly is essential. Look for these signs:
- Sudden collapse with no response to shouting or tapping
- No normal breathing (watch for agonal breathing, which is irregular gasping that may look like the person is breathing but is actually a sign of cardiac arrest)
- No pulse detected
- Loss of consciousness within seconds
If you witness these signs, call 911 immediately, begin CPR, and retrieve the nearest AED. The combination of CPR and early defibrillation is the most effective way to save a life during SCA. For a step-by-step guide, see how to use an AED.
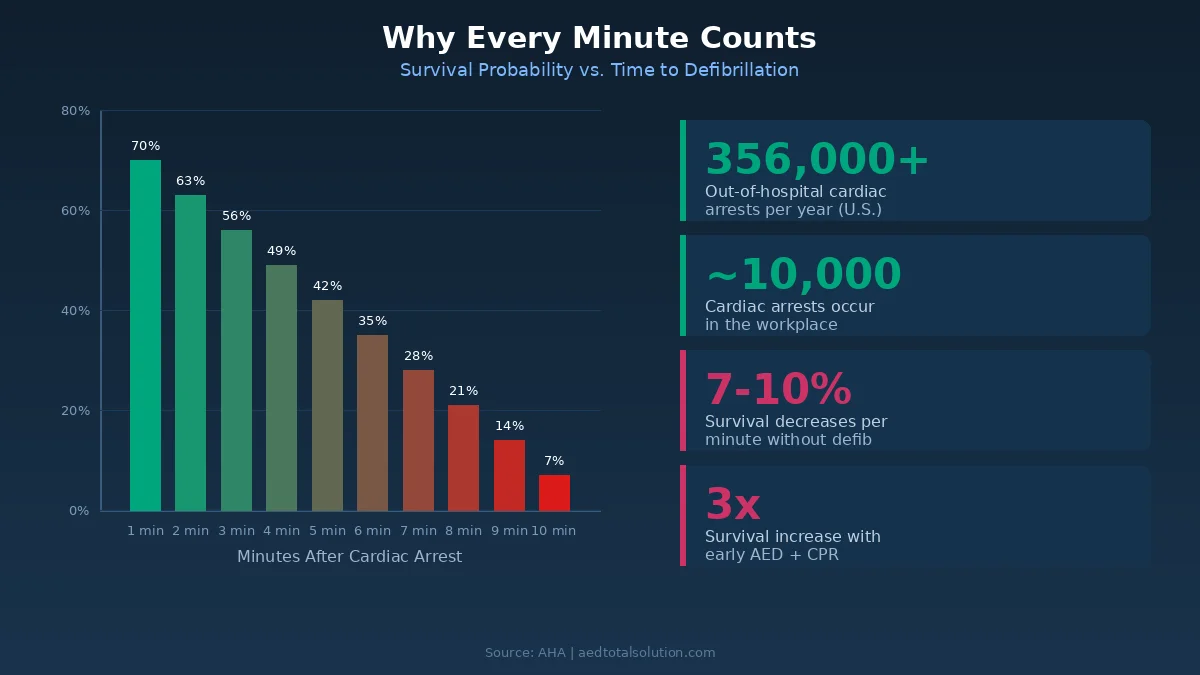
Why Workplaces Need Defibrillators
OSHA recommends that all workplaces include AEDs as part of their first-aid and emergency preparedness programs. While OSHA does not currently mandate AEDs at the federal level, several states have enacted their own AED requirements by state, and many industries are moving toward mandatory AED programs.
The case for workplace defibrillators is compelling:
- Time is the critical factor. Average EMS response time in the U.S. is 7 to 14 minutes. For every minute without defibrillation, survival probability drops by 7% to 10%. An on-site AED can deliver a shock within 1 to 3 minutes of a cardiac arrest.
- SCA happens at work. Approximately 10,000 cardiac arrests occur in the workplace each year. Employees over 45, those with cardiovascular risk factors, and individuals in physically demanding roles are at elevated risk.
- AEDs are proven to save lives. Studies in the New England Journal of Medicine have shown that public-access AED programs double the survival rate for out-of-hospital cardiac arrest.
- Legal protection exists. Good Samaritan laws in all 50 states provide legal protection for bystanders who use an AED in good faith during an emergency.
Organizations with multiple locations face additional complexity in maintaining AED compliance across sites. Our multi-location AED compliance guide explains how to manage this effectively.
How to Choose the Right AED for Your Organization
Selecting an AED involves more than picking a device off a shelf. Consider these factors:
Key Selection Criteria
- Semi-automatic vs. fully automatic: Semi-automatic AEDs require the user to press a button to deliver a shock, giving them a moment of control. Fully automatic models deliver the shock without user intervention. For environments where responders may hesitate (such as schools), fully automatic models may be preferable.
- Pediatric capability: If children are present (schools, daycares, family recreation centers), choose an AED with pediatric mode or compatible pediatric AED pads.
- Ruggedness and IP rating: For outdoor, construction, or industrial environments, look for AEDs with higher IP (ingress protection) ratings for dust and water resistance.
- Total cost of ownership: AED costs go beyond the purchase price. Factor in battery replacements, electrode pad replacements, maintenance, training, and compliance tracking. Our AED pricing guide breaks down all the costs.
- Program management needs: For organizations with multiple devices, centralized tracking of maintenance schedules, pad and battery expiration dates, and compliance documentation becomes essential. AED program management services handle this operational burden.
Need help choosing? Browse our AED selection or request a quote for a customized recommendation based on your facility size, risk profile, and budget.
AED Maintenance and Compliance
Owning an AED is only the first step. Keeping it ready to perform when needed requires ongoing maintenance and regulatory compliance.
Essential AED Maintenance Tasks
- Monthly visual inspections: Check the status indicator light, verify pads and batteries are not expired, and confirm the device is accessible and properly mounted. See our AED inspection frequency guide for detailed schedules.
- Electrode pad replacement: Most AED pads expire every 2 to 5 years, depending on the manufacturer. Expired pads may not adhere properly or conduct the electrical shock effectively. Learn more about AED pad expiration and replacement.
- Battery replacement: AED batteries typically last 2 to 5 years in standby mode. Our AED battery life guide explains what affects battery longevity and when to replace.
- Compliance documentation: Many states require AED registration, regular inspections, and documentation. Our AED compliance management guide covers the requirements by state.
For organizations that want hands-off compliance, AED Total Solution’s managed services provide automated monitoring, supply replacement scheduling, physician oversight, and audit-ready documentation.
AED Training and Certification
While no state in the U.S. requires formal training to use an AED in an emergency, training builds confidence and improves response times. Trained bystanders are significantly more likely to take action during a cardiac emergency.
Common AED training programs include:
- AHA Heartsaver CPR AED: A widely recognized 4-hour course covering CPR, AED use, and choking relief
- American Red Cross First Aid/CPR/AED: A comprehensive course available online and in-person
- Workplace-specific training: Many AED program providers offer on-site training tailored to your organization’s devices and emergency action plan
For a detailed comparison of training options, costs, and AED certification requirements, see our complete training guide.
The History of Defibrillators
Defibrillation is not a new concept. Understanding its history helps illustrate why modern AEDs represent such an important advancement in public health.
- 1899: Physiologists Jean-Louis Prevost and Frederic Batelli discovered that electrical shocks could induce and reverse ventricular fibrillation in animals.
- 1947: Dr. Claude Beck performed the first successful human defibrillation at Case Western Reserve University during open-chest surgery.
- 1956: Dr. Paul Zoll performed the first closed-chest defibrillation, eliminating the need for surgery to deliver a shock.
- 1960s: Dr. Frank Pantridge developed the first portable defibrillator for use in ambulances in Belfast, Northern Ireland, earning him the title “Father of Emergency Medicine.”
- 1979: The first automatic external defibrillator was developed by Drs. Arch Diack, Robert Rullman, and W. Stanley Welborn, making it possible for non-physicians to perform defibrillation.
- 2000s–present: Public-access AED programs have expanded dramatically. Today, AEDs are found in airports, schools, workplaces, sports venues, and homes. Modern AEDs weigh as little as 2.5 pounds and cost a fraction of what earlier models did.
Frequently Asked Questions About Defibrillators
What does a defibrillator do?
A defibrillator delivers a controlled electrical shock to the heart to restore a normal rhythm during sudden cardiac arrest. It interrupts chaotic electrical activity (ventricular fibrillation or pulseless ventricular tachycardia) so the heart can resume effective pumping.
Can anyone use an AED?
Yes. AEDs are designed for use by anyone, regardless of medical training. The device provides step-by-step voice instructions, and built-in safety features prevent a shock from being delivered unless it is needed. All 50 states provide Good Samaritan legal protection for AED users.
Is a defibrillator the same as a pacemaker?
No. A defibrillator delivers a shock to stop dangerous arrhythmias, while a pacemaker delivers small, regular electrical impulses to maintain a steady heartbeat. An ICD combines defibrillator and pacemaker functions in one implanted device. See our full comparison of defibrillator vs. pacemaker.
How much does a defibrillator cost?
AEDs for public and workplace use typically cost between $1,200 and $3,000. Total cost of ownership, including pads, batteries, maintenance, and compliance management, can add $200 to $500 per year. See our complete AED pricing guide.
Why is defibrillation important?
Defibrillation is important because it is the only effective treatment for ventricular fibrillation, the most common cause of sudden cardiac arrest. CPR alone cannot restart a heart in VF. Early defibrillation, combined with CPR, can increase survival rates from less than 10% to nearly 70%.
How does a defibrillator work on the heart?
A defibrillator sends an electrical current through the heart muscle via electrode pads on the chest. This current simultaneously depolarizes all heart muscle cells, stopping the chaotic electrical activity. After this “reset,” the heart’s natural pacemaker can re-establish a normal, coordinated rhythm.
Do I need an AED in my workplace?
OSHA recommends AEDs for all workplaces. Several states legally require them in certain facilities. Even where not mandated, the evidence strongly supports having AEDs: they reduce workplace cardiac arrest mortality significantly. Check our guide on AED laws by state to see what applies to your location.
What is the difference between an AED and a defibrillator?
An AED is a type of defibrillator. The term “defibrillator” covers all devices that deliver shocks to the heart, including manual defibrillators (used by doctors), ICDs (implanted), and WCDs (wearable). An AED is specifically the automated, portable type designed for public use. For a more detailed breakdown, see our article on AED vs. defibrillator.
Take Action: Protect Your Organization with an AED Program
Every minute without defibrillation during sudden cardiac arrest reduces survival by up to 10%. Having the right defibrillator in the right place, maintained and ready, is not just a best practice; it is a responsibility.
AED Total Solution provides full-service AED program management, from device selection and installation to ongoing compliance monitoring and physician oversight. Whether you need a single AED for a small office or a multi-site program for an enterprise organization, we deliver a white-glove solution that keeps your team protected and your compliance documentation audit-ready.
Ready to get started? Request a free quote or call us to speak with an AED program specialist. You can also browse our AED inventory to compare FDA-approved devices from leading manufacturers.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• ResponseReady.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.


