-
 Written By
Prabakar Mahalingam
Written By
Prabakar Mahalingam
- Published
ICD vs. Pacemaker: Key Differences, How They Work, and What You Need to Know

Both implantable cardioverter defibrillators (ICDs) and pacemakers are life-saving cardiac devices, but they treat very different heart conditions. A pacemaker keeps your heart from beating too slowly. An ICD prevents sudden cardiac arrest by detecting and correcting dangerously fast or irregular heart rhythms. This guide explains how each device works, when doctors recommend one over the other, and what to expect if you or someone in your organization needs one.
What Is a Pacemaker?
A pacemaker is a small, battery-powered device implanted under the skin near the collarbone. It monitors your heart rate and sends gentle electrical pulses through thin wires (called leads) whenever the heart beats too slowly or pauses.
Pacemakers treat bradycardia, a condition where the heart rate drops below 60 beats per minute and causes symptoms like fatigue, dizziness, or fainting. The device activates only when needed, and most people never feel the low-energy pulses it delivers.
Types of Pacemakers
There are several pacemaker configurations, each designed for specific heart conditions:
- Single-chamber pacemaker — One lead connects to either the right atrium or right ventricle, stimulating one chamber of the heart.
- Dual-chamber pacemaker — Two leads connect to the right atrium and right ventricle, coordinating contractions between both chambers.
- Biventricular pacemaker (CRT-P) — Three leads connect to the right atrium, right ventricle, and left ventricle. Used for cardiac resynchronization therapy in patients with heart failure.
- Leadless pacemaker — A small, self-contained capsule placed directly inside the heart during a catheter-based procedure. No chest incision or leads required.
Common Conditions Treated by Pacemakers
Doctors typically recommend a pacemaker for:
- Sinus node dysfunction (sick sinus syndrome)
- Atrioventricular (AV) block (second-degree or complete heart block)
- Bradycardia causing fatigue, dizziness, or syncope
- Chronotropic incompetence (inability to increase heart rate during activity)
What Is an ICD (Implantable Cardioverter Defibrillator)?
An implantable cardioverter defibrillator, or ICD, is a device that continuously monitors heart rhythm and delivers electrical therapy when it detects life-threatening arrhythmias. While it looks similar to a pacemaker and is implanted the same way, an ICD has a critical additional capability: it can deliver high-energy shocks to reset the heart during ventricular tachycardia or ventricular fibrillation.
Many modern ICDs also include pacemaker functions, meaning they can treat slow heart rhythms with low-energy pacing in addition to responding to dangerous fast rhythms with stronger shocks.
What Does AICD Stand For?
You may see the term AICD (automatic implantable cardioverter defibrillator) used interchangeably with ICD. AICD was the original name for the device when it was first developed in the 1980s. Today, most medical professionals simply use “ICD,” though both terms refer to the same type of device.
Types of ICDs
- Single-chamber ICD — One lead connects to the right ventricle. Monitors and treats ventricular arrhythmias.
- Dual-chamber ICD — Two leads connect to the right atrium and right ventricle. Allows the device to distinguish between atrial and ventricular rhythms more accurately.
- Biventricular ICD (CRT-D) — Three leads coordinate the heart’s chambers while also providing defibrillation. Used for patients with heart failure who also need protection from sudden cardiac arrest.
- Subcutaneous ICD (S-ICD) — The lead is placed under the skin near the heart rather than threaded through veins. Avoids lead-related vascular complications but cannot provide anti-tachycardia pacing.
Common Conditions Treated by ICDs
Doctors typically recommend an ICD for:
- Survivors of cardiac arrest (secondary prevention)
- Patients with left ventricular ejection fraction (LVEF) ≤35% and heart failure (primary prevention)
- Sustained ventricular tachycardia with structural heart disease
- Hypertrophic cardiomyopathy with high risk of sudden cardiac death
- Long QT syndrome or Brugada syndrome with documented risk factors
ICD vs. Pacemaker: Key Differences at a Glance
Understanding the core differences between these devices helps clarify why your doctor may recommend one over the other.
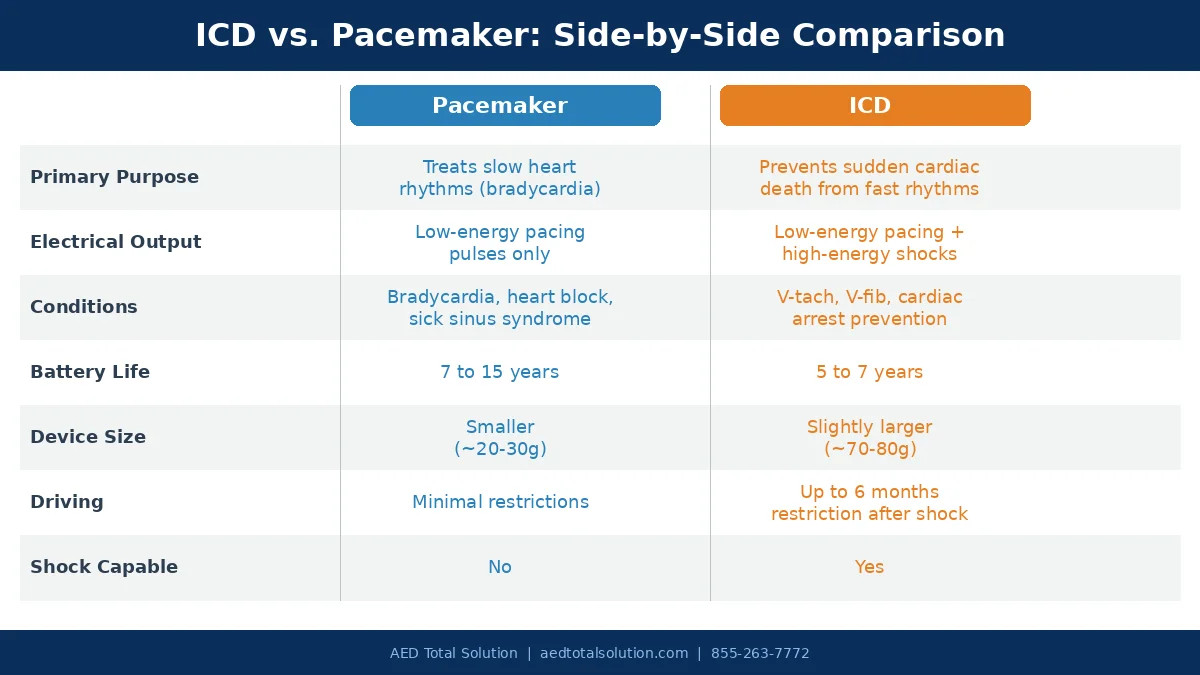
| Feature | Pacemaker | ICD |
|---|---|---|
| Primary purpose | Treats slow heart rhythms (bradycardia) | Prevents sudden cardiac death from fast, dangerous rhythms |
| Electrical output | Low-energy pacing pulses | Low-energy pacing + high-energy defibrillation shocks |
| Conditions treated | Bradycardia, heart block, sick sinus syndrome | Ventricular tachycardia, ventricular fibrillation, cardiac arrest risk |
| Shocking capability | No | Yes |
| Pacing capability | Yes | Yes (most modern ICDs include pacemaker functions) |
| Battery life | 7 to 15 years | 5 to 7 years |
| Implantation | Minor surgery, local anesthesia | Minor surgery, local anesthesia (similar to pacemaker) |
| Driving restrictions | Minimal | May be restricted for up to 6 months |
How Does Each Device Work?
How a Pacemaker Works
A pacemaker continuously monitors heart rate. When it detects a beat that is too slow or a pause in rhythm, it sends a small electrical impulse through the leads to stimulate the heart muscle and maintain an adequate heart rate.
Modern pacemakers are “demand” devices, meaning they only activate when the heart needs help. If your natural rhythm is normal, the pacemaker stays silent. This preserves battery life and reduces unnecessary pacing.
How an ICD Works
An ICD monitors every heartbeat, similar to a pacemaker. However, when it detects a dangerously fast or chaotic rhythm, it responds with one of three therapies:
- Anti-tachycardia pacing (ATP) — A series of rapid, low-energy pulses that may interrupt the fast rhythm and restore normal beating without a shock. Most patients do not feel this.
- Cardioversion — A moderate-energy shock delivered when ATP is not effective. May feel like a thump in the chest.
- Defibrillation — A high-energy shock that resets the heart’s electrical system during ventricular fibrillation. Often described as a sudden kick to the chest, but lasts only a fraction of a second.
In most cases, a single shock restores normal rhythm. If someone experiences multiple shocks in a short period (an “electrical storm”), they should seek emergency medical attention immediately.
Can You Have Both a Pacemaker and an ICD?
Yes. Many patients need help with both slow and fast heart rhythms. Rather than implanting two separate devices, doctors typically use a combination device that integrates pacemaker and ICD functions into a single unit.
CRT-D (Cardiac Resynchronization Therapy Defibrillator) devices are the most common combination. They coordinate the heart’s chambers to improve pumping efficiency (like a biventricular pacemaker) while also providing defibrillation protection against sudden cardiac arrest.
Your cardiologist or electrophysiologist will determine whether a standalone device or combination device is appropriate based on your specific heart condition, ejection fraction, and risk factors.
Life Expectancy and Outcomes
Both pacemakers and ICDs significantly improve quality of life and can extend life expectancy for patients with the conditions they treat.
Research shows that ICDs reduce the risk of sudden cardiac death substantially. For patients with heart failure and reduced ejection fraction, ICDs have demonstrated a significant reduction in mortality compared to medication alone.
Pacemakers, meanwhile, relieve symptoms of bradycardia and can restore normal activity levels. Many patients with pacemakers live long, full lives with minimal restrictions.
For a deeper look at survival rates and what to expect after device implantation, read our guide on life expectancy after ICD implant.
Living with a Pacemaker or ICD: What to Expect
Recovery After Implantation
Both devices are implanted through a similar minor surgical procedure:
- A small incision is made near the collarbone under local anesthesia with sedation.
- Leads are threaded through a vein into the heart (except for leadless pacemakers and S-ICDs).
- The device generator is placed in a pocket under the skin.
- The device is tested and programmed before closing the incision.
Most patients go home the same day or the next day. Recovery typically involves:
- 2 to 4 weeks of activity restrictions (no heavy lifting, overhead movements, or strenuous exercise)
- Avoiding contact sports permanently (to protect the device)
- Gradual return to normal activities as directed by your cardiologist
Long-Term Precautions
After the initial recovery period, most people with pacemakers or ICDs resume normal daily life. Key precautions include:
- Cell phones — Keep at least 6 inches away from the device.
- MRI scans — Many newer devices are MRI-conditional, but always inform your healthcare team.
- Airport security — Carry your device identification card. Request a manual pat-down if preferred.
- Magnets and high-voltage equipment — Maintain a safe distance to avoid electromagnetic interference.
- Medical procedures — Always inform all healthcare providers (doctors, dentists, technicians) that you have an implanted device.
Remote Monitoring
Modern pacemakers and ICDs support remote monitoring, allowing your care team to check device performance, battery life, and heart rhythm data without requiring an office visit. Regular in-person checkups (typically every 6 to 12 months) complement remote monitoring to ensure optimal device function.
ICDs, Pacemakers, and the Role of External Defibrillators (AEDs)
While ICDs protect individual patients from sudden cardiac arrest, automated external defibrillators (AEDs) protect everyone else in a cardiac emergency. Approximately 356,000 out-of-hospital cardiac arrests occur in the United States each year, and the majority happen to people who do not have an implanted device.
Organizations that deploy AEDs alongside cardiac emergency response plans create safer environments for employees, visitors, and the public. Understanding the difference between internal devices (ICDs, pacemakers) and external devices (AEDs) is part of building a comprehensive approach to sudden cardiac arrest preparedness.
Key distinctions:
- ICDs are implanted in high-risk patients and activate automatically from inside the body.
- AEDs are portable, public-access devices designed for bystander use during a cardiac emergency.
- A person with an ICD can still benefit from an AED if their device fails to restore a normal rhythm or if the battery is depleted.
If your organization is evaluating emergency preparedness equipment, contact AED Total Solution to learn how a managed AED program can protect your workforce. Our AED rental program provides an affordable way to get started with FDA-approved devices from $45/month. Call us at 855-263-7772 for a free consultation.
Frequently Asked Questions
What is the main difference between an ICD and a pacemaker?
A pacemaker treats slow heart rhythms (bradycardia) by sending low-energy electrical pulses to keep the heart beating at an adequate rate. An ICD is designed to prevent sudden cardiac death by detecting and correcting dangerously fast or irregular heart rhythms with electrical shocks. Most modern ICDs also include pacemaker capabilities.
Is an ICD the same as a pacemaker?
No. While both are implanted cardiac devices, they serve different purposes. A pacemaker prevents the heart from beating too slowly, while an ICD prevents sudden cardiac arrest caused by ventricular tachycardia or ventricular fibrillation. Some combination devices perform both functions.
What does AICD stand for?
AICD stands for automatic implantable cardioverter defibrillator. It is the original term for what is now commonly called an ICD. Both terms describe the same type of device.
Can someone with a pacemaker or ICD use an AED?
Yes. If a person with an implanted device experiences cardiac arrest and their device is not restoring a normal rhythm, bystanders should still use an AED. Place the AED pads at least 1 inch away from the implanted device and follow the AED’s voice prompts as normal.
How long do pacemakers and ICDs last?
Pacemaker batteries typically last 7 to 15 years, while ICD batteries last 5 to 7 years. When the battery is low, the generator is replaced through a minor outpatient procedure. The leads usually remain in place.
Can you drive with an ICD or pacemaker?
Pacemaker patients can typically resume driving within a few days of implantation if cleared by their doctor. ICD patients may face driving restrictions of up to 6 months after implantation or after the device delivers a shock. Commercial driver’s licenses (CDL) are generally not permitted for ICD patients. Always follow your cardiologist’s guidance.
Disclaimer: This article is for educational and informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for diagnosis and treatment of any heart condition.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• ResponseReady.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.

