Sudden cardiac arrest and heart attack are two of the most misunderstood medical emergencies. Many people use the terms interchangeably, but they are fundamentally different conditions with different causes, symptoms, and treatments. Understanding the difference between cardiac arrest and heart attack is not just medical trivia. It can mean the difference between life and death when seconds count.
This guide breaks down what sudden cardiac arrest (SCA) and heart attack are, how to recognize each, and why having an automated external defibrillator (AED) nearby is one of the most important steps any organization can take to protect lives.
Key Takeaway: Sudden cardiac arrest is an electrical malfunction where the heart stops beating suddenly, while a heart attack is a circulation problem caused by a blocked artery. Both are emergencies, but they require different responses.
- Cardiac arrest causes immediate collapse; the only treatment is CPR and AED defibrillation
- Heart attack symptoms develop gradually; treatment restores blood flow via medical intervention
- A heart attack can lead to cardiac arrest, but they are not the same condition
- Survival from cardiac arrest drops 7-10% per minute without defibrillation
- Having an AED on site and knowing how to use it can increase survival rates to over 70%
What Is Sudden Cardiac Arrest?
Sudden cardiac arrest is an electrical malfunction of the heart. During SCA, the heart’s electrical system misfires, causing the heart to suddenly stop beating effectively. This typically happens due to an arrhythmia called ventricular fibrillation, where the heart quivers rapidly instead of pumping blood.
When the heart stops pumping, blood flow to the brain, lungs, and other vital organs ceases immediately. Without intervention, a person in cardiac arrest will lose consciousness within seconds and can suffer permanent brain damage or death within minutes.
Key facts about sudden cardiac arrest:
- According to the American Heart Association (AHA), more than 356,000 out-of-hospital cardiac arrests occur in the United States each year.
- Approximately 10,000 cardiac arrests happen in workplaces annually, according to the Occupational Safety and Health Administration (OSHA).
- SCA can strike anyone, at any age, often without prior warning signs.
- Only about 10% of people who experience out-of-hospital cardiac arrest survive, largely due to delayed response times.
What Is a Heart Attack?
A heart attack, also known as a myocardial infarction, is a circulation problem. It occurs when a blocked artery prevents oxygen-rich blood from reaching a section of the heart muscle. If the blockage is not treated quickly, the part of the heart muscle that is deprived of blood begins to die.
Unlike sudden cardiac arrest, the heart usually continues to beat during a heart attack. However, the longer the blockage remains, the more damage the heart muscle sustains.
Common causes of heart attack include:
- Coronary artery disease (plaque buildup in the arteries)
- Blood clots that form at the site of a ruptured plaque
- Coronary artery spasm (less common)
Heart attacks often develop over time as a result of risk factors like high blood pressure, high cholesterol, smoking, diabetes, obesity, and family history of heart disease.
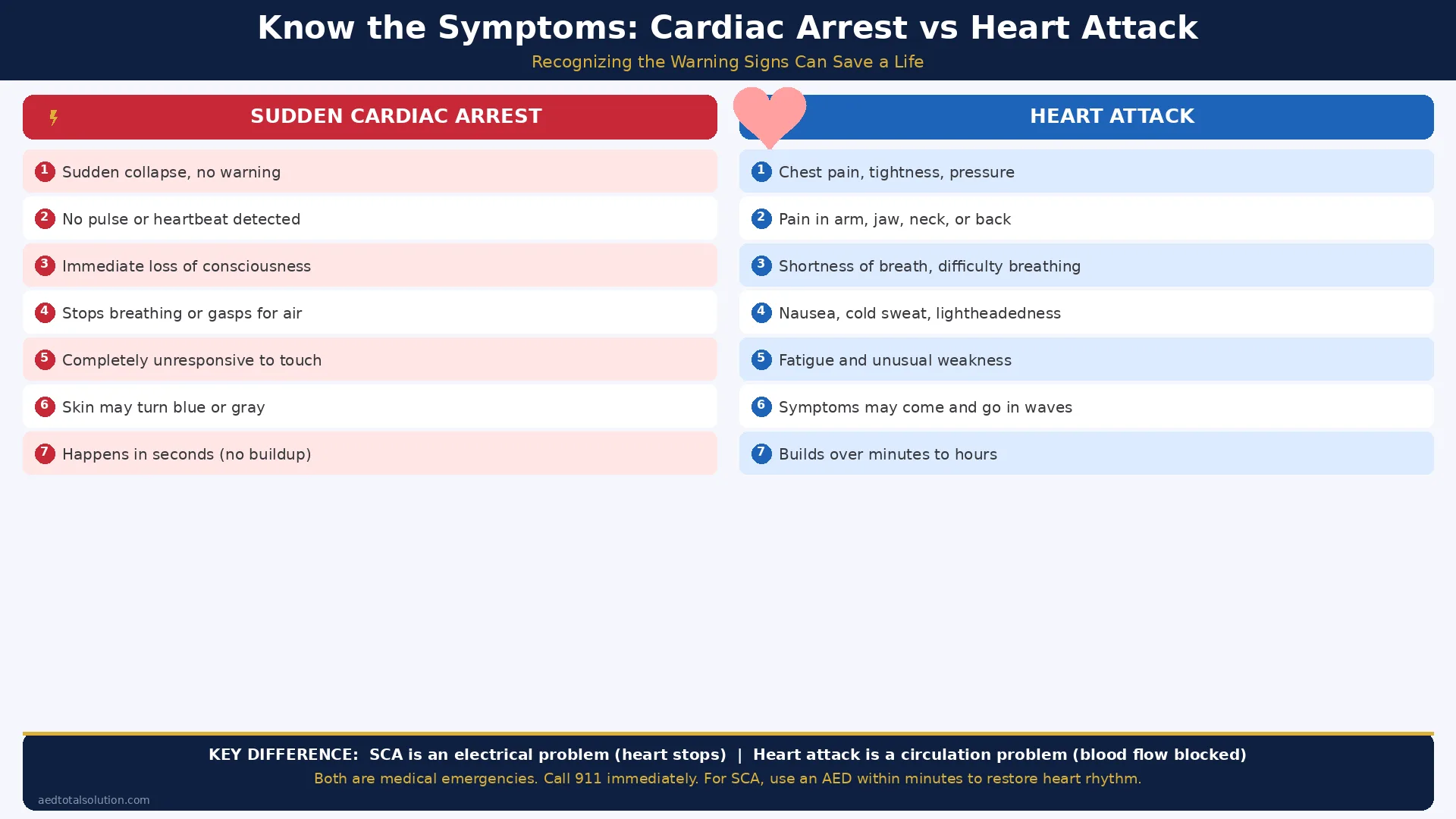
Cardiac Arrest vs Heart Attack: A Side-by-Side Comparison
Understanding the differences at a glance can help you respond appropriately in an emergency.
| Feature | Sudden Cardiac Arrest | Heart Attack |
|---|---|---|
| What it is | An electrical malfunction; the heart stops beating | A circulation blockage; blood flow to heart muscle is cut off |
| Onset | Sudden, without warning | Symptoms can develop over hours, days, or weeks |
| Consciousness | Person collapses and becomes unresponsive within seconds | Person is usually conscious and aware |
| Breathing | Stops breathing or only gasps | Breathing may be labored but typically continues |
| Pulse | No detectable pulse | Pulse is usually present |
| Primary treatment | Immediate CPR and AED defibrillation | Emergency medical care to restore blood flow (medications, angioplasty, stenting) |
| Can one cause the other? | A heart attack can trigger cardiac arrest | Cardiac arrest does not cause a heart attack |
Signs and Symptoms of Cardiac Arrest
Cardiac arrest symptoms strike suddenly with little to no warning. Recognizing these signs of cardiac arrest immediately is critical because every second counts:
- Sudden collapse with loss of consciousness
- No pulse or heartbeat detectable
- No breathing or only abnormal gasping
- Unresponsiveness to stimulation
In some cases, a person may experience brief warning signs in the minutes before cardiac arrest, including dizziness, chest discomfort, shortness of breath, or heart palpitations. However, many cardiac arrests occur without any prior symptoms.
Signs and Symptoms of a Heart Attack
Heart attack symptoms typically develop more gradually and can range from mild to severe. Recognizing these signs early and seeking medical attention can prevent a heart attack from progressing to cardiac arrest.
Common heart attack symptoms include:
- Chest pain, pressure, tightness, or a squeezing sensation
- Pain that radiates to the arm, jaw, neck, back, or stomach
- Shortness of breath (with or without chest discomfort)
- Cold sweats, nausea, or lightheadedness
- Unusual fatigue (especially in women)
It is important to note that heart attack symptoms can present differently in women, older adults, and people with diabetes. Women are more likely to experience atypical symptoms such as back pain, jaw pain, nausea, and extreme fatigue rather than classic chest pain.
What Causes Cardiac Arrest?
Understanding cardiac arrest causes helps identify who may be at risk. The most common causes include:
- Ventricular fibrillation (V-fib): The most frequent trigger, where the heart’s lower chambers quiver chaotically instead of pumping.
- Heart attack: A severe heart attack can damage the heart’s electrical system and trigger cardiac arrest.
- Cardiomyopathy: Thickened or enlarged heart muscle that affects electrical conduction.
- Heart valve disease: Malfunctioning valves that strain the heart and can cause arrhythmias.
- Congenital heart defects: Structural abnormalities present from birth.
- Long QT syndrome and other inherited conditions: Genetic disorders affecting the heart’s electrical activity.
- External factors: Severe trauma, drug overdose, drowning, electrocution, or extreme physical exertion can all trigger cardiac arrest.
Who Is at Risk?
While sudden cardiac arrest can happen to anyone, certain factors increase the risk:
- Prior heart conditions: coronary artery disease, heart failure, previous heart attack, or arrhythmia history
- Age: Risk increases with age, particularly after 45 for men and 55 for women
- Family history: A family history of cardiac arrest or sudden cardiac death
- Lifestyle factors: Smoking, excessive alcohol use, drug use, sedentary lifestyle, and obesity
- Underlying health conditions: Diabetes, high blood pressure, high cholesterol, and kidney disease
Organizations with higher-risk populations, such as fitness centers, manufacturing facilities, schools, and offices with employees over 40, should be especially proactive about having AEDs on site and a comprehensive AED program management plan.
What to Do When Someone Experiences Sudden Cardiac Arrest
Immediate action during cardiac arrest is the single most important factor in survival. The AHA’s Chain of Survival outlines the critical steps:
Step 1: Recognize and Call 911
If someone suddenly collapses, is unresponsive, and is not breathing normally, assume cardiac arrest. Call 911 immediately or direct someone nearby to call.
Step 2: Start CPR Immediately
Begin high-quality chest compressions at a rate of 100-120 compressions per minute, pressing at least 2 inches deep on the center of the chest. If trained, alternate 30 compressions with 2 rescue breaths. If untrained, perform hands-only CPR. For more information, read our guide on CPR and AED guide.
Step 3: Use an AED as Soon as Possible
An automated external defibrillator (AED) is a portable device that delivers an electric shock to restore the heart’s normal rhythm. AEDs are designed for use by anyone, even without medical training. For details, see our guide on automated external defibrillators (AEDs). The device provides voice prompts that guide the user through each step.
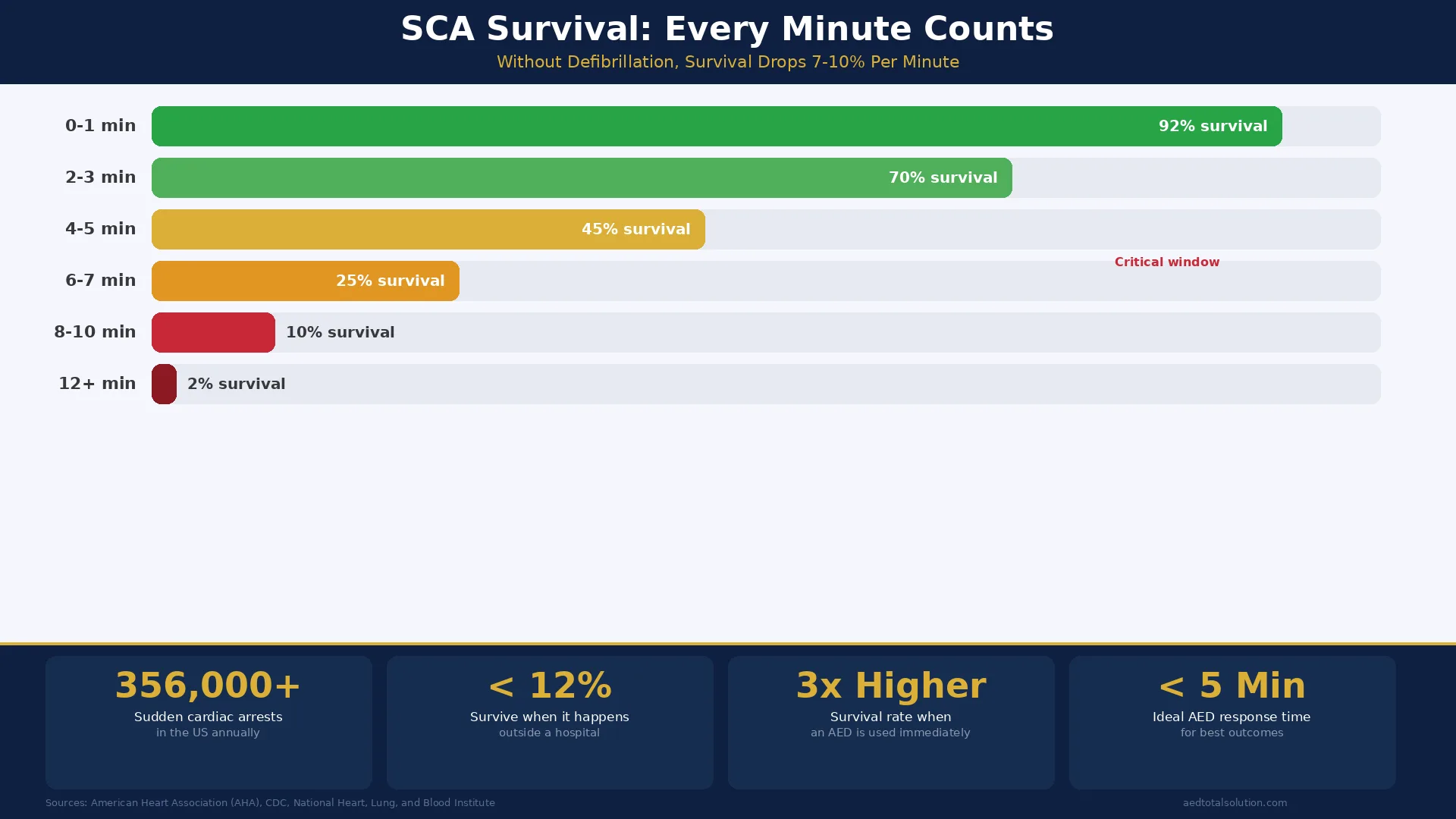
Why AEDs are critical for SCA survival:. For more information, read our guide on cardiac arrest survival rates.
- Survival chances decrease by 7 to 10% for every minute that passes without defibrillation, according to the AHA.
- When an AED is used within the first few minutes of cardiac arrest, survival rates can reach 70% or higher.
- Bystander CPR combined with early AED use can triple the chances of survival compared to waiting for emergency medical services.
- Without defibrillation, only about 5 to 7% of cardiac arrest victims survive to hospital discharge.
Step 4: Advanced Medical Care
Emergency medical services provide advanced life support, including medications, advanced airway management, and transport to the hospital for further treatment.
Why Every Workplace Needs an AED Program
Given that approximately 10,000 cardiac arrests occur in workplaces each year (OSHA), organizations have both a moral and practical obligation to be prepared. OSHA recommends that employers implement AED programs as part of their workplace safety plans.
However, simply purchasing an AED is not enough. AEDs require ongoing maintenance, including regular battery and electrode pad replacement, routine inspections, proper placement, and staff training. An expired battery or depleted electrode pad can render an AED useless during an emergency.
This is where a managed AED program makes the difference. AED Total Solution provides comprehensive, white-glove AED program management that covers:
- AED selection and placement guidance tailored to your facility layout
- Registration and compliance documentation to meet OSHA guidance and state requirements
- Routine inspections and readiness verification so devices are always response-ready
- Battery and pad lifecycle tracking with proactive replacement reminders
- Remote readiness monitoring through a centralized compliance dashboard
- Audit-ready reporting for regulatory reviews and internal compliance audits
- Scalable solutions for multi-location organizations managing devices across multiple sites
Whether your organization is deploying its first AED or managing a fleet of devices across multiple locations, AED Total Solution simplifies compliance while strengthening your emergency preparedness.
How to Reduce Your Risk: Prevention Strategies
While not all cardiac arrests or heart attacks can be prevented, the following strategies can significantly reduce risk:
-
Schedule regular health screenings. Monitor blood pressure, cholesterol, and blood sugar levels. Early detection of heart disease risk factors allows for timely intervention.
-
Maintain a heart-healthy lifestyle. Eat a balanced diet rich in fruits, vegetables, whole grains, and lean proteins. Limit sodium, saturated fats, and processed foods.
-
Exercise regularly. The CDC recommends at least 150 minutes of moderate-intensity aerobic activity per week for adults.
-
Quit smoking. Smoking is one of the leading preventable risk factors for both heart attack and cardiac arrest.
-
Manage chronic conditions. Work with your healthcare provider to control high blood pressure, diabetes, high cholesterol, and other conditions that increase cardiac risk.
-
Know your family history. If you have a family history of heart disease, sudden cardiac death, or arrhythmias, talk to your doctor about screening and prevention options. For high-risk patients, an implantable cardioverter-defibrillator (ICD) may be recommended.
-
Learn CPR and how to use an AED. Bystander intervention is the most critical factor in cardiac arrest survival. Ensure your workplace has accessible AEDs and trained responders.
-
Implement a workplace AED program. Organizations that invest in a managed AED program ensure their people and facilities are prepared for cardiac emergencies at all times.
Frequently Asked Questions
Is cardiac arrest the same as a heart attack?
No. Cardiac arrest is an electrical malfunction that causes the heart to stop beating suddenly. A heart attack is a blockage that reduces blood flow to the heart muscle. They are different conditions, though a heart attack can sometimes trigger cardiac arrest.
Can you survive sudden cardiac arrest?
Yes, but survival depends on how quickly treatment begins. Immediate CPR and AED use within the first few minutes can dramatically increase survival rates. Without intervention, survival rates drop by 7 to 10% for every minute that passes.
What is the survival rate for cardiac arrest?
The overall survival rate for out-of-hospital cardiac arrest is approximately 10%, according to the AHA. However, when bystanders perform CPR and use an AED promptly, survival rates can exceed 70%.
Do AEDs really save lives?
Absolutely. AEDs are the only effective treatment for ventricular fibrillation, the most common cause of sudden cardiac arrest. Early defibrillation, combined with CPR, is the single greatest factor in cardiac arrest survival.
Does OSHA require AEDs in the workplace?
While OSHA does not currently mandate AEDs in all workplaces, OSHA strongly recommends that employers include AED programs as part of their emergency action plans. Many states have additional AED requirements for specific facility types.
How does AED Total Solution help with AED compliance?
AED Total Solution provides full-service AED program management, including device selection, placement, registration, inspections, monitoring, battery and pad tracking, and compliance documentation. Our managed approach ensures your AEDs are always response-ready and your program meets OSHA guidance and state requirements.
This article is for informational and educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. If you or someone near you is experiencing symptoms of a heart attack or cardiac arrest, call 911 immediately.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• ResponseReady.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.




