Reviewed by Prabakar Mahalingam, Managing Partner at AED Total Solution. Prabakar is a renowned national provider of safety training, products, and proprietary compliance software dedicated to addressing Sudden Cardiac Arrest (SCA).
If you have ever searched “AED vs defibrillator,” you are not alone. The two terms are often used interchangeably, which creates real confusion for safety officers, HR leaders, and business owners trying to make informed decisions about workplace emergency preparedness. Here is the short answer: an AED is a type of defibrillator. The word “defibrillator” is the broad category, while an AED (Automated External Defibrillator) is one specific type designed for use by everyday people with no medical training. Understanding this distinction matters because choosing the right device, maintaining it properly, and meeting compliance requirements all depend on knowing exactly what you are working with.
Key Takeaways: A defibrillator is any device that delivers an electrical shock to restore a normal heart rhythm. An AED is a specific type of defibrillator built for public use, with automated heart rhythm analysis and step-by-step voice prompts. Manual defibrillators are reserved for trained medical professionals in hospitals and ambulances. For workplaces, schools, and public facilities, an AED is the correct device to purchase and maintain. AED Total Solution provides full-service AED program management to keep your devices compliant and response-ready.
What Is a Defibrillator?
A defibrillator is a medical device that delivers a controlled electrical shock to the heart. The purpose of this shock is to interrupt an abnormal heart rhythm, known as an arrhythmia, and allow the heart to reset to its normal electrical pattern. Defibrillators treat life-threatening conditions like ventricular fibrillation (VF) and pulseless ventricular tachycardia (VT), both of which cause the heart to stop pumping blood effectively.
The concept has existed since the 1940s, when external defibrillation was first performed in a clinical setting. Since then, the technology has evolved from large hospital machines into multiple device categories designed for different users, settings, and levels of medical training.
The word “defibrillator” is an umbrella term that covers several distinct device types. Understanding these categories is the first step to answering the question of AED vs defibrillator.
Types of Defibrillators: A Complete Breakdown
There are four main categories of defibrillators used today. Each serves a different purpose and is designed for a different user.

1. Automated External Defibrillators (AEDs)
An AED is a portable, battery-powered device designed for use by the general public. When someone experiences sudden cardiac arrest (SCA), a bystander can turn on the AED, attach the adhesive electrode pads to the person’s chest, and follow the device’s voice prompts. The AED automatically analyzes the heart rhythm and determines whether a shock is needed. If it detects a shockable rhythm, it either delivers the shock automatically (fully automatic models) or prompts the user to press a button (semi-automatic models).
The critical safety feature of an AED is that it will not deliver a shock unless it detects a life-threatening rhythm. This makes it impossible for a bystander to accidentally harm someone, which is why AEDs are placed in offices, schools, airports, gyms, and other public spaces.
Popular AED brands include Philips HeartStart, ZOLL AED 3, HeartSine Samaritan, Defibtech Lifeline, and Cardiac Science Powerheart. Prices for new AEDs typically range from $1,200 to $2,500 depending on features and accessories. Browse available options on our AED shop page.
2. Manual External Defibrillators
Manual defibrillators are the devices you see in hospitals and on ambulances. Unlike AEDs, they require the operator to read an ECG (electrocardiogram) display, interpret the heart rhythm, select the appropriate energy level (measured in joules), and manually trigger the shock. These devices also offer additional clinical functions such as synchronized cardioversion, external pacing, and multi-lead cardiac monitoring.
Examples include the LIFEPAK 15, ZOLL X Series, and Philips HeartStart MRx. They cost between $10,000 and $35,000 and are used exclusively by paramedics, emergency physicians, nurses, and other trained healthcare providers.
3. Implantable Cardioverter-Defibrillators (ICDs)
An ICD is a small device surgically placed inside the chest of patients at high risk for dangerous heart rhythms. It continuously monitors the heart and delivers an internal shock when it detects ventricular fibrillation or ventricular tachycardia. ICDs are prescribed by cardiologists and are a long-term treatment, not an emergency response tool. They are not the same as pacemakers, although some combination devices (CRT-D) include both pacing and defibrillation functions.
4. Wearable Cardioverter-Defibrillators (WCDs)
A WCD, such as the ZOLL LifeVest, is a vest-like device worn externally by patients who are temporarily at high risk for sudden cardiac arrest but are not yet candidates for an ICD implant. It monitors the heart continuously and delivers a shock through electrode pads built into the vest if a dangerous rhythm is detected.
AED vs Defibrillator: Key Differences at a Glance
The core distinction between an AED and other defibrillators comes down to three factors: who uses it, where it is used, and how much training is required.
| Feature | AED (Automated External Defibrillator) | Manual Defibrillator |
|---|---|---|
| Intended user | General public, any bystander | Trained medical professionals only |
| Training required | Minimal to none; voice prompts guide use | Advanced cardiac life support (ACLS) certification |
| Heart rhythm analysis | Automated by the device | Operator reads and interprets ECG |
| Shock delivery | Automated or single-button press | Operator selects energy level and timing |
| Typical setting | Offices, schools, gyms, airports, public buildings | Hospitals, ambulances, emergency departments |
| Cost | $1,200 to $2,500 | $10,000 to $35,000 |
| Size and portability | 2 to 7 lbs, highly portable | 15 to 30 lbs, mounted on carts or walls |
| Additional functions | CPR coaching (some models), event recording | Cardioversion, pacing, multi-lead ECG monitoring |
| Maintenance | Monthly visual checks, pad/battery replacement every 2 to 5 years | Biomedical engineering maintenance schedule |
How Does a Defibrillator Work?
All defibrillators work on the same fundamental principle. When the heart enters ventricular fibrillation, its electrical signals become chaotic, causing the heart muscle to quiver instead of pumping blood. A defibrillator delivers a controlled dose of electrical energy through the chest wall (or internally, in the case of ICDs) that momentarily stops all electrical activity in the heart. This brief pause gives the heart’s natural pacemaker, the sinoatrial (SA) node, a chance to regain control and reestablish a normal rhythm.
The difference between device types lies in how that shock is controlled:
- AEDs use built-in algorithms to analyze the heart rhythm and determine the correct energy level. The user does not make clinical decisions.
- Manual defibrillators display the heart rhythm on a screen. The healthcare provider interprets the rhythm, selects the joule level (typically 120 to 360 joules for adults), and decides when to deliver the shock.
- ICDs are programmed by a cardiologist to detect specific arrhythmia patterns and deliver a pre-set shock internally.
For workplaces and public settings, an AED’s automated approach is the safest and most practical option. No ECG interpretation skills are needed, and the device will not deliver a shock unless it is medically appropriate.
Is a Defibrillator the Same as a Pacemaker?
No. This is one of the most common misconceptions. A pacemaker and a defibrillator serve different purposes:
- A pacemaker treats a heart that beats too slowly (bradycardia). It delivers small, continuous electrical impulses to keep the heart beating at a steady rate.
- A defibrillator (specifically an ICD) treats a heart that beats dangerously fast or chaotically (ventricular fibrillation or ventricular tachycardia). It delivers a high-energy shock to reset the rhythm.
Some patients receive a combination device called a CRT-D (Cardiac Resynchronization Therapy Defibrillator) that provides both pacing and defibrillation. But the devices address fundamentally different electrical problems in the heart.
For workplace safety planning, this distinction is important: an AED is an external emergency device, not a replacement for or related to implanted pacemakers. A person with a pacemaker can still experience sudden cardiac arrest and may still need an AED.
Who Uses Each Type of Defibrillator?
Understanding who operates each type of defibrillator helps clarify why an AED is the right choice for non-clinical environments:
- AEDs: Office employees, school staff, coaches, gym personnel, security guards, event coordinators, flight attendants, and any bystander. No medical license required.
- Manual defibrillators: Emergency physicians, paramedics, EMTs (in some jurisdictions), critical care nurses, and other ACLS-certified healthcare providers.
- ICDs: Prescribed and implanted by cardiologists for individual patients. Not a workplace device.
- WCDs: Prescribed by a physician for patients awaiting an ICD or recovering from a cardiac event. Worn by the individual patient.
The bottom line for businesses: if you are evaluating whether your workplace needs a defibrillator, the answer is almost always an AED. Manual defibrillators require clinical expertise your staff does not have, and implantable devices are patient-specific medical treatments.
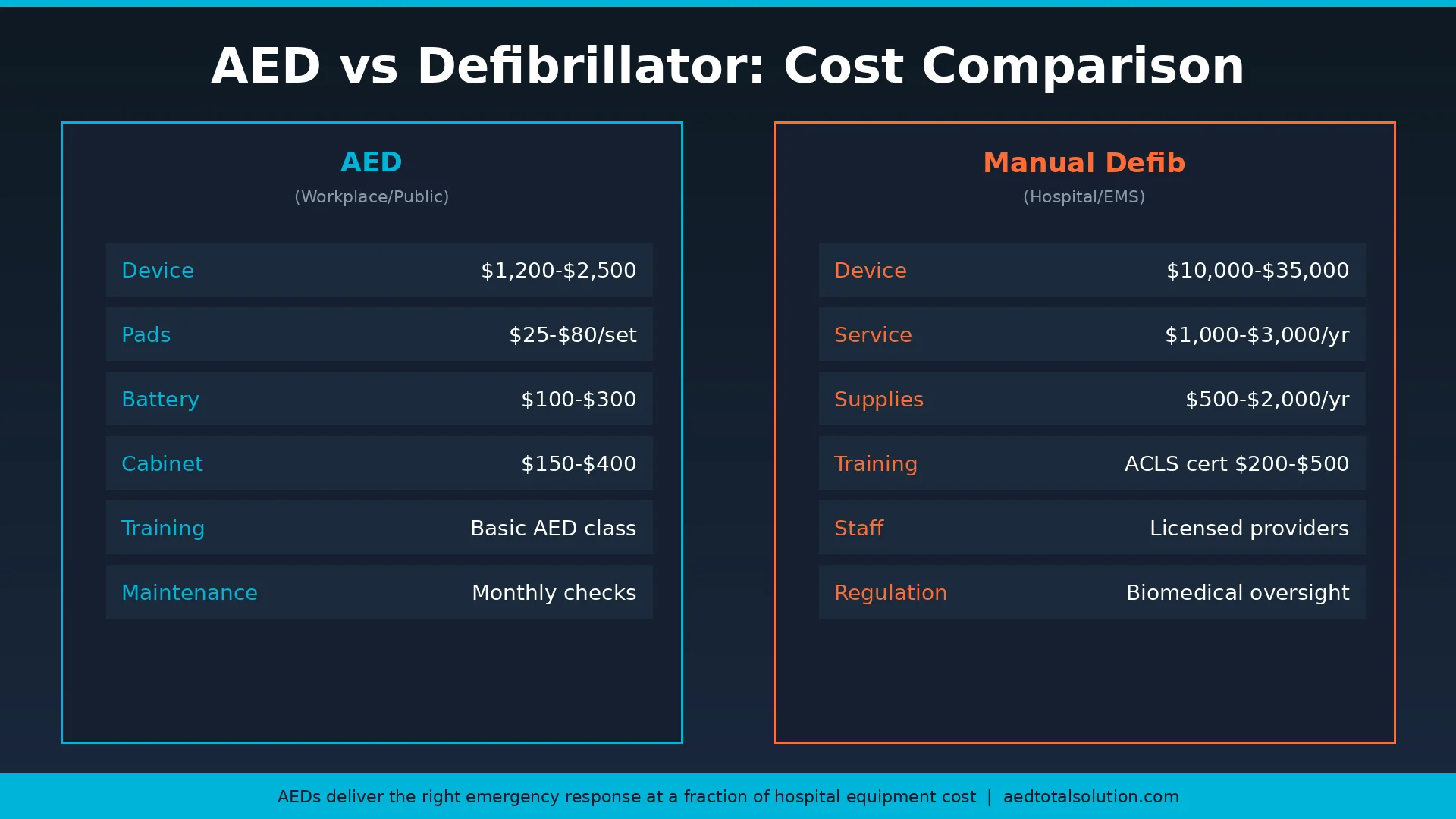
AED Cost vs Manual Defibrillator Cost
Cost is one of the most practical differences between AEDs and manual defibrillators. Here is a realistic breakdown:
AED Costs (Workplace/Public Access)
- Device: $1,200 to $2,500 for new FDA-cleared models
- Replacement pads: $25 to $80 per set, replaced every 2 to 5 years
- Replacement battery: $100 to $300, replaced every 4 to 5 years
- Cabinet and signage: $150 to $400
- Annual program management: Varies by provider; includes inspections, compliance tracking, and documentation
Organizations that need AEDs temporarily, such as for events or construction sites, can also consider AED rental programs as a cost-effective alternative.
Manual Defibrillator Costs (Hospital/EMS)
- Device: $10,000 to $35,000
- Annual service contracts: $1,000 to $3,000
- Accessories and consumables: $500 to $2,000 per year
- Training: ACLS certification courses ($200 to $500 per provider, renewed every 2 years)
For businesses, schools, and public facilities, AEDs deliver the right level of cardiac emergency response at a fraction of the cost of clinical equipment.
Workplace and Public Access AED Requirements
Many states have laws requiring AEDs in specific settings. While OSHA does not currently mandate AEDs, it has published guidance encouraging employers to include AEDs in workplace first-aid programs. The American Heart Association (AHA) recommends that AEDs be available within 3 to 5 minutes of any location where people gather.
State-level requirements vary significantly:
- California: Health studios and fitness facilities must have AEDs on-site. Learn more in our California AED requirements guide.
- New York: Public schools, health clubs, and certain public buildings are required to have AEDs and trained staff.
- Most states: Good Samaritan protections apply to bystanders who use an AED in good faith during an emergency.
For a complete overview, see our AED requirements by state guide.
Compliance goes beyond simply purchasing a device. An effective AED program requires regular inspections, pad and battery tracking, staff awareness, proper placement, and documentation that proves readiness. This is where managed AED program services become essential, especially for organizations with devices across multiple locations.
Choosing the Right Defibrillator for Your Organization
For the vast majority of non-clinical organizations, the decision is straightforward: you need an AED. Here is a quick decision framework:
- Workplace, school, gym, or public facility: AED (automated external defibrillator). No medical training required for use. Staff should receive basic AED awareness or CPR/AED training.
- Hospital, ambulance, or emergency department: Manual defibrillator operated by ACLS-certified providers.
- Individual patient with diagnosed arrhythmia: ICD or WCD as prescribed by a cardiologist.
When selecting an AED for your organization, consider these factors:
- Semi-automatic vs fully automatic: Fully automatic AEDs deliver the shock without a button press, which can reduce hesitation from untrained rescuers.
- CPR feedback: Models like the ZOLL AED 3 provide real-time compression depth and rate coaching.
- Pediatric capability: If children are present, choose a model with an easy pediatric mode (Philips FRx Infant/Child Key or HeartSine Pediatric Pad-Pak).
- Connectivity: WiFi-enabled AEDs allow remote readiness monitoring, reducing the burden of manual inspections.
- Total cost of ownership: Include pads, batteries, cabinets, training, and ongoing compliance management in your budget.
Not sure where to start? Our team can help you evaluate your needs and build a fully managed AED program that covers device selection, placement, maintenance, and compliance documentation.
Frequently Asked Questions
Is an AED the same as a defibrillator?
An AED is a type of defibrillator, but not all defibrillators are AEDs. The term “defibrillator” covers multiple device types including AEDs, manual defibrillators, ICDs, and wearable defibrillators. An AED is specifically designed for public use with automated features that make it safe for anyone to operate during a cardiac emergency.
Can a regular person use a defibrillator?
A regular person can use an AED, which is the type of defibrillator designed for bystander use. AEDs provide voice prompts and automated heart rhythm analysis. Manual defibrillators, however, require advanced medical training and should only be operated by healthcare professionals.
Is a defibrillator and a pacemaker the same thing?
No. A pacemaker treats a slow heartbeat by delivering small electrical impulses to maintain a steady rhythm. A defibrillator treats a dangerously fast or chaotic heartbeat by delivering a high-energy shock. Some implantable devices combine both functions, but they address different cardiac conditions.
How much does an AED cost compared to a hospital defibrillator?
AEDs for workplace and public access use typically cost $1,200 to $2,500. Manual defibrillators used in hospitals and ambulances range from $10,000 to $35,000. AEDs provide the appropriate level of emergency response for non-clinical settings at a fraction of the cost.
Does OSHA require workplaces to have defibrillators?
OSHA does not currently mandate AEDs in the workplace, but it has published guidance encouraging employers to include AEDs as part of a comprehensive workplace first-aid program. Many individual states have laws requiring AEDs in specific settings such as fitness centers, schools, and large public buildings.
What should I do after purchasing an AED?
Purchasing the AED is only the first step. You need to register the device with local EMS, establish an inspection schedule, track pad and battery expiration dates, train staff on basic AED use, place the device in an accessible location with proper signage, and maintain documentation for compliance audits. A managed AED program handles all of these requirements through a single provider.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• ResponseReady.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.




