An Automated External Defibrillator is a sophisticated medical device, not just another piece of safety equipment like a fire extinguisher. Because it delivers a medical treatment, it requires clinical expertise to ensure it’s used safely and effectively. Simply hanging it on the wall ignores the critical medical and legal requirements that come with it, such as needing a physician’s prescription to own one in the first place. A truly effective program needs this clinical expertise at its core. This is why AED program management with medical direction is not just a best practice, but often a legal necessity. It ensures your emergency protocols are sound, your device is properly maintained, and your program is built on a solid clinical foundation.
Key Takeaways
- Treat your AED as a complete safety system: An effective program goes beyond the device itself, requiring consistent team training, routine inspections, and organized documentation to ensure you’re always prepared.
- Physician oversight is essential for compliance and safety: Medical direction is a non-negotiable requirement in many states that ensures your program follows clinical best practices, protecting both your people and your organization from risk.
- Proactive management prevents failure: Consistently tracking expiration dates, performing inspections, and maintaining audit-ready records are the keys to guaranteeing your AED is functional and your program remains compliant over time.
What is AED Program Management and Medical Direction?
Deciding to get an AED for your workplace is a fantastic first step toward protecting your team and visitors. But a truly effective program involves more than just mounting a box on the wall. That’s where AED program management comes in. Think of it as the complete operational system that ensures your device is ready to go at a moment’s notice and that your organization is fully compliant with all the rules. It covers everything from selecting the right AED and deciding where to place it, to performing routine inspections, tracking expiration dates for pads and batteries, and training your team. A well-managed program removes the guesswork and anxiety from AED ownership.
A critical piece of this puzzle is Medical Direction, or medical oversight. This might be a new term for you, but it’s a non-negotiable part of a compliant and effective program. It means having a licensed physician oversee your entire AED setup. They provide the necessary medical expertise to ensure your program not only meets legal standards but also follows clinical best practices. This partnership between hands-on management and expert AED program management services are designed to handle all of these details for you, giving you total peace of mind.
Understanding the Role of a Medical Director
A Medical Director is a licensed physician who acts as the official supervisor for your AED program. In many states, this isn’t just a good idea—it’s the law. This doctor provides the necessary medical oversight to ensure everything is done correctly from a clinical standpoint. They are responsible for writing the prescription required to purchase an AED, which is something many people are surprised to learn. Beyond the initial prescription, they help establish emergency response protocols, ensure your device is registered with local EMS, and provide guidance on how to properly use the AED. Think of them as your program’s dedicated medical expert, ensuring every step you take is sound, safe, and effective.
Why Compliance is Non-Negotiable
When it comes to your AED program, compliance isn’t just about checking a box on a form—it’s about protecting people and your organization. Failing to follow local, state, and federal regulations can have serious consequences. First and foremost, a non-compliant device may fail during an emergency, turning a life-saving opportunity into a tragedy. From a legal perspective, non-compliance can expose your organization to significant liability and lawsuits, where it can be presented as evidence of negligence. A solid, compliant AED program is your best defense. It demonstrates that you’ve taken every necessary step to prepare for a sudden cardiac arrest event, ensuring your equipment is ready and your procedures are sound.
Why is Medical Direction a Must-Have for Your AED Program?
When you decide to place an AED in your facility, you’re making a commitment to protecting the people in your building. But simply mounting a device on the wall isn’t enough. A truly effective AED program operates under medical direction, which means a licensed physician oversees every aspect of it, from the initial setup to post-event review. Think of it as having a medical expert on your team who ensures your program is not only compliant but also clinically sound and ready to save a life.
This oversight is the foundation of a responsible and defensible program. It moves your AED from being just a piece of equipment to being part of an integrated emergency response system. Without it, you’re left guessing about complex medical and legal requirements, which can create serious gaps in your preparedness. A comprehensive program management service integrates medical direction seamlessly, giving you confidence that every detail is handled correctly. It’s about ensuring your good intentions are backed by expert guidance, so your AED is always ready when seconds matter most.
Meeting State Requirements
One of the most critical reasons for medical direction is simple: it’s often the law. Many states have specific statutes that require a physician to oversee any AED program. These laws are in place to ensure that life-saving devices are implemented safely and effectively under professional medical guidance. A medical director provides the necessary prescription for the AED (which is a medical device regulated by the FDA) and verifies that your program aligns with all state and local regulations. This oversight helps you avoid fines and penalties associated with non-compliance, but more importantly, it confirms your program is built on a solid, legally sound foundation from day one.
Protecting Your Organization from Liability
In the event of a sudden cardiac arrest, a non-compliant or poorly managed AED program can become a major liability. If a device fails due to improper maintenance or if protocols aren’t followed correctly, your organization could face devastating legal consequences. Medical direction is one of your strongest tools for risk management. Having a physician oversee your program demonstrates a clear commitment to quality and due diligence. This expert oversight ensures your devices are properly maintained, your team is trained, and your response protocols follow established best practices, significantly reducing your organization’s liability exposure and creating a safer environment for everyone.
Ensuring Clinical Best Practices
Beyond legal compliance, medical direction ensures your program is clinically effective. A medical director helps you make crucial decisions based on established medical guidelines, such as where to place AEDs for the fastest response time and what training your team needs. They also play a vital role after an AED is used. The physician will review the event data, provide feedback to your responders, and coordinate with local EMS. This post-event review is essential for quality assurance and continuous improvement. It provides your team with valuable support and confirms your program is always ready to provide the best possible care in an emergency.
What Makes Up a Complete AED Program?
A truly effective AED program is much more than a device hanging on a wall. It’s a complete system designed to ensure your organization is ready to respond to a sudden cardiac arrest emergency. Think of it as having four core pillars: smart device selection and placement, thorough team training, consistent readiness checks, and diligent documentation. When all these pieces work together, you create a program that not only meets compliance standards but also builds genuine confidence that you’re prepared for the moments that matter most. A well-structured AED program management plan addresses every one of these components, turning a simple piece of equipment into a life-saving asset.
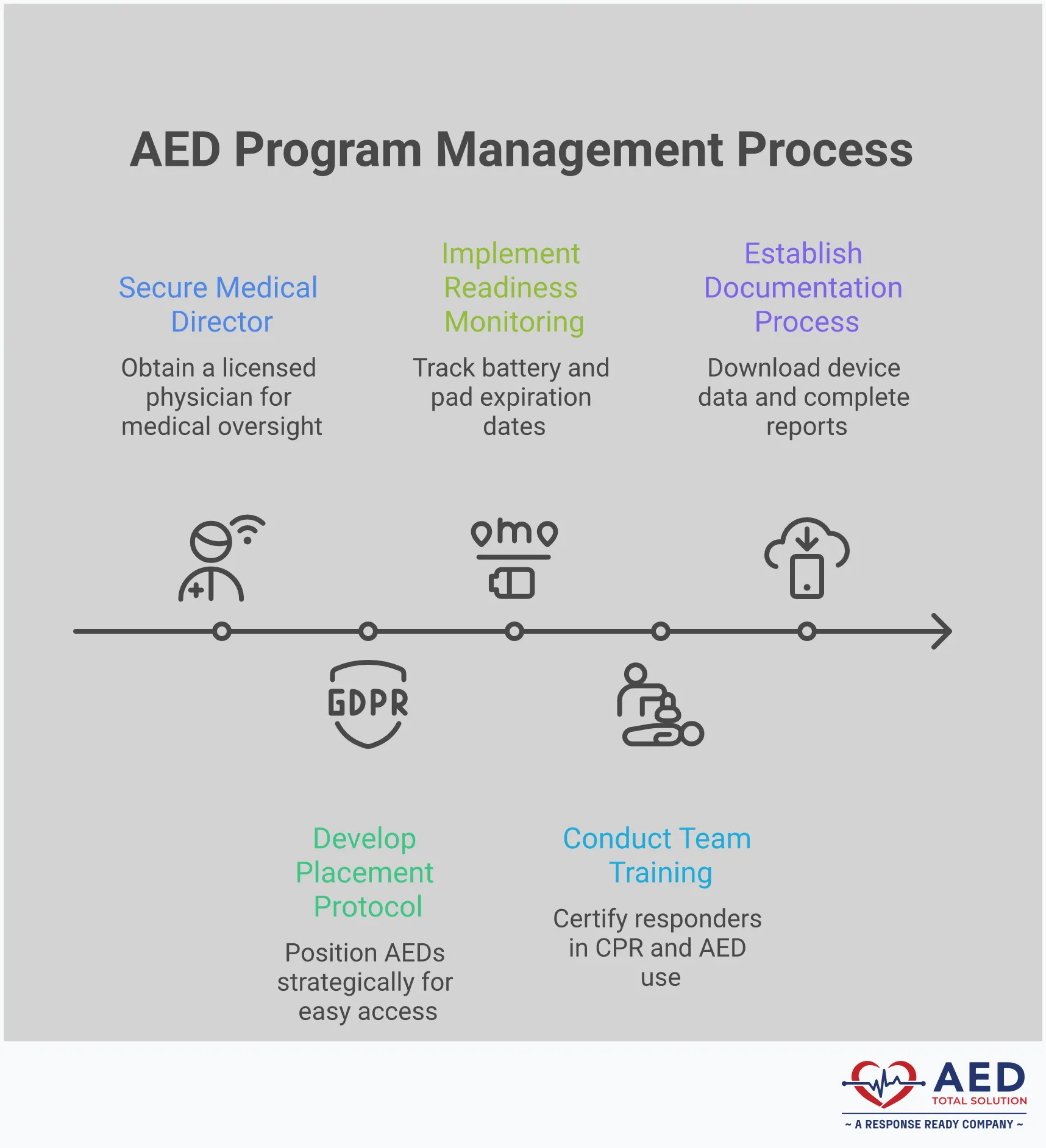
Choosing and Placing Your AEDs
Deciding where to install your AEDs is a critical first step that requires careful thought. The goal is to place them in visible, accessible locations where they can be retrieved and used within three minutes of a collapse. As OSHA guidance suggests, every workplace should assess its unique needs, considering factors like building layout, employee count, and high-risk areas. This process isn’t just about finding an empty wall; it involves getting physician oversight to ensure the plan is clinically sound and coordinating with local EMS to align with community response protocols. Proper placement is the foundation of a rapid and effective emergency response.
Training and Certifying Your Team
An AED is only as effective as the people who use it. That’s why comprehensive training is a non-negotiable part of any successful program. Your designated responders should be certified in both CPR and AED use, as these skills are used together to give a person the best chance of survival. Effective AED training goes beyond the basics of turning the device on; it builds the confidence and situational awareness your team needs to act decisively in a high-stress emergency. When people feel prepared, they are far more likely to step in and help when seconds count.
Keeping Your Devices Ready
An AED program requires ongoing attention to keep it functional. This means assigning a person or team to perform routine maintenance and inspections. These checks involve confirming the device is operational, ensuring pads and batteries have not expired, restocking supplies, and staying on top of any manufacturer recalls or software updates. Without consistent oversight, it’s easy for a device to become unusable without anyone realizing it until it’s too late. These routine inspections are the only way to guarantee your AED is ready to perform when called upon.
Handling Documentation and Reporting
Proper documentation is the backbone of a compliant and defensible AED program. Most states require you to register your device with local EMS and provide them with follow-up data after it’s used in an emergency. This reporting helps first responders and improves the chain of survival in your community. Keeping detailed records of your device maintenance, team training certifications, and readiness checks ensures you are always audit-ready. This paperwork isn’t just red tape; it’s proof that you are managing your program responsibly and are committed to protecting the people in your care.
What Does Medical Direction Actually Cover?
When you hear “medical direction,” you might picture a doctor simply signing off on a form. But it’s so much more than a signature. True medical direction is the clinical backbone of your entire AED program, providing the medical expertise and oversight needed to ensure your program is safe, effective, and compliant. It’s what transforms a box on the wall into a life-saving tool integrated with a clear emergency plan. A dedicated medical director oversees every clinical aspect, from device prescriptions to post-event analysis, making sure your team is prepared to respond correctly when it matters most. This comprehensive oversight is a core part of our AED program management services.
Think of it this way: buying an AED is like buying a fire extinguisher. You have the tool, but you also need a plan. Who uses it? When? How do you ensure it works? Medical direction provides that plan for your AED. It ensures your program is built on a solid clinical foundation, meeting all state and federal regulations while following best practices for emergency response. A medical director doesn’t just write a prescription; they help you build a culture of preparedness. They ensure your response protocols are sound, your team is confident, and your program can withstand scrutiny after an event. It’s this active, ongoing involvement that protects your organization and, most importantly, gives a person in cardiac arrest the best possible chance of survival.
Physician Oversight and Prescriptions
Because an Automated External Defibrillator (AED) is a medical device, you can’t just buy one and hang it on the wall. The FDA classifies AEDs as Class III medical devices, which require a physician’s prescription to own and operate. This is where medical direction begins. A licensed physician acts as your program’s medical director, providing the necessary prescription for each device. This oversight ensures your program is established correctly from a medical and legal standpoint. Many states have specific laws that require this physician oversight for an organization to be protected by Good Samaritan laws, making it a critical first step in responsible AED ownership.
Developing Your Emergency Protocols
What happens the moment someone collapses? Who calls 911? Who retrieves the AED? A medical director helps you answer these questions by developing clear and effective emergency response protocols. These are the specific, step-by-step rules your team will follow to provide patient care during a sudden cardiac arrest event. This plan is customized to your facility’s layout, staff roles, and unique needs. Having a physician-approved protocol removes guesswork during a high-stress emergency, ensuring your team can act quickly and confidently. It provides a clear framework for everything from initial response to handing off care to professional EMS responders.
Reviewing Events to Improve Response
After an AED is used, the work isn’t over. A crucial part of medical direction is the post-event review. The medical director helps your team download the event data stored by the AED, which includes details about the patient’s heart rhythm and the shocks delivered. The physician reviews this information and provides constructive feedback to your response team. This process helps identify what went well and where there are opportunities for improvement in future responses. This continuous quality improvement loop is essential for maintaining a high standard of care and ensuring your team’s skills stay sharp.
Coordinating with Local EMS
Your AED program doesn’t operate in a vacuum—it’s the first link in the chain of survival. Medical direction ensures your program is properly integrated with your local Emergency Medical Services (EMS). Most states require you to register your AEDs with the local 911 dispatch and coordinate your response plan with them. Your medical director can manage this communication, ensuring first responders know where your AEDs are located. After an event, they also handle providing the necessary follow-up data to EMS, closing the loop and contributing to better community-wide cardiac arrest outcomes. This coordination is a key piece of maintaining AED compliance.
Common Roadblocks in AED Program Management
Even with the best intentions, managing an AED program can feel like a full-time job. You’re juggling device maintenance, team training, and a stack of compliance paperwork, all while handling your actual day-to-day responsibilities. It’s easy for critical details to slip through the cracks. Most organizations run into the same handful of challenges, but recognizing them is the first step to building a program that runs smoothly and effectively. From shifting regulations to the simple logistics of tracking multiple devices, these common hurdles can compromise your program’s readiness if left unaddressed. Let’s walk through the biggest roadblocks you might face and how to think about clearing them.
Keeping Up with Changing Rules
AED laws aren’t uniform; they vary significantly by state and sometimes even by city. These regulations cover everything from where an AED must be placed to who needs to be notified of its location. Staying on top of these rules is a constant challenge, as they can be updated with little notice. Failing to meet these requirements isn’t just a paperwork problem—it can create serious liability issues and, more importantly, could mean your AED isn’t ready when needed. A solid AED program management plan must include a process for monitoring and adapting to these legislative changes to ensure your organization remains fully compliant and protected.
Maintaining Staff Readiness and Awareness
Placing an AED on the wall is only half the battle. Your team needs the confidence and skills to act decisively in an emergency. This means providing comprehensive training that covers both AED operation and CPR. But training isn’t a one-time event. Certifications expire, and skills get rusty. A common roadblock is failing to track and schedule refresher courses, leading to a decline in team readiness over time. An effective program includes ongoing education and regular drills to ensure that when an emergency happens, your responders can step in without hesitation and perform their roles effectively.
Meeting Medical Oversight Demands
Many states require that an AED program be supervised by a licensed physician. This medical director is responsible for writing a prescription for the device, reviewing protocols, and ensuring the program follows clinical best practices. For many organizations, finding a physician to take on this role and understanding what it entails can be a major hurdle. This isn’t just a box to check; medical oversight is a critical component that validates your program’s procedures and provides an essential layer of quality control. It ensures your emergency response plan is sound, defensible, and aligned with current medical standards.
Managing AEDs Across Multiple Locations
As your organization grows, so does the complexity of your AED program. Tracking one device is simple enough, but what about ten devices across three states? Each AED has its own set of batteries and pads with different expiration dates, its own inspection schedule, and its own local registration requirements. Without a centralized system, it’s incredibly easy to lose track, leaving some locations with an expired or non-functional device. This logistical challenge is one of the biggest risks for multi-site organizations, making a unified AED management solution essential for maintaining readiness and compliance across the board.
How to Choose the Right Program Management Partner
Selecting a partner to manage your AED program is one of the most important decisions you’ll make to protect your organization and its people. This isn’t just about buying a device; it’s about entrusting a critical safety function to an expert who can handle the details, from compliance to clinical oversight. A great partner acts as an extension of your team, giving you confidence that your program is always ready for an emergency. As you evaluate your options, focus on a few key areas: the quality of their medical direction, their track record with compliance, the services they actually provide, and the technology they use to keep your AEDs response-ready. Getting these things right from the start will save you headaches and significantly reduce your organization’s liability.
Check the Medical Director’s Credentials
Any legitimate AED program management service will have a medical director, but not all medical oversight is created equal. This physician is legally and ethically responsible for your program, so you need to know who they are and what their qualifications are. Having a doctor oversee your AED program is a strong way to manage risks and ensure quality. Don’t be afraid to ask direct questions. Is their medical director licensed to practice in your state? What is their background in emergency medicine? A partner should be transparent about their medical leadership, as it’s the foundation of a clinically sound and defensible program.
Verify Their Compliance Record
Compliance is the backbone of a safe and effective AED program. When a program isn’t compliant, the consequences can be severe—non-compliant organizations face the risk of AED failures that can lead to avoidable deaths and lawsuits. A prospective partner should be able to demonstrate a strong history of keeping clients compliant with all federal, state, and local regulations. Ask for references or case studies from organizations similar to yours. A trustworthy partner will not only understand current laws but will also proactively track legislative changes to ensure your program never falls out of compliance. They should make it easy for you to prove your program is audit-ready at all times.
Understand the Scope of Service and Support
The term “program management” can mean different things to different providers, so it’s crucial to understand exactly what you’re paying for. A comprehensive service should cover every aspect of the AED lifecycle, from initial placement and registration to ongoing maintenance and post-event support. True AED program management helps you stay compliant and prepared. Look for a partner that offers automated alerts for battery and pad expirations, regular inspection tracking, and detailed documentation. The goal is to find a solution that removes the administrative burden from your team while ensuring your devices are always ready to save a life.
Review Their Monitoring Technology
In the past, managing multiple AEDs meant relying on manual checklists and calendar reminders—a system prone to human error. Today, technology has changed the game. Leading program management partners use remote monitoring to automate readiness checks. This technology can confirm that an AED is in its proper location and that its status indicator is green, signaling it’s ready for use. An AED program paired with remote monitoring can also reduce costs, especially for organizations with devices across multiple locations. Ask potential partners to demonstrate their software and explain how it provides real-time visibility into your program’s health.
Understanding the Cost of AED Program Management
When you start looking into AED program management, you’ll find that the costs are more than just a line item on a budget. Think of it as an investment in safety, compliance, and peace of mind. A great program handles all the complex details—from medical oversight to readiness checks—so you can focus on running your organization, confident that your emergency response plan is solid. The price you pay covers the expertise and systems needed to keep your AEDs ready and your program compliant, which is a small price for knowing you’re prepared for a sudden cardiac arrest emergency. Let’s break down what you can expect to pay and, more importantly, the value you get in return.
Breaking Down Service Pricing
Most AED program management services are priced on a per-device, per-year basis, which makes it easy to scale your program whether you have one AED or one hundred. A typical plan that includes medical direction and compliance management often starts around $150 per year for a single device. Many providers also offer multi-year subscriptions, which can lower the annual cost and simplify your budgeting for the long term. This fee isn’t just for a piece of software; it covers the ongoing support, physician oversight, and automated tracking that ensures your device is always ready to use and that you meet all state and local requirements.
What to Watch For: Hidden Fees
The most significant costs associated with an AED program aren’t on the price list—they’re the hidden risks of going it alone. Without proper management, you could face serious consequences. An AED that fails during an emergency because of an expired battery or pad can lead to devastating outcomes and potential lawsuits. Non-compliance with registration and maintenance laws can also be used as evidence of negligence. A comprehensive AED program management service is designed to prevent these issues, protecting your organization from liability while ensuring your team is truly prepared to save a life. The real “hidden fee” is the cost of not being ready when it matters most.
Calculating Your Return on Investment
The return on investment for AED program management goes far beyond dollars and cents. First, there’s the peace of mind that comes from knowing your program is fully compliant and your devices are monitored by experts. This frees up your team from the administrative burden of tracking expiration dates, logging inspections, and staying on top of changing regulations. With a physician providing medical oversight, you also add a layer of clinical credibility to your program, ensuring you’re following best practices. Ultimately, the ROI is measured in readiness. A well-managed program gives you confidence that your AED will work as intended, which is an invaluable return when a life is on the line.
How to Keep Your Program Effective for the Long Haul
Deploying an AED is a fantastic first step, but it’s not the last one. An effective AED program is a living system that requires consistent attention to ensure it’s ready to go at a moment’s notice. Think of it less like a one-time purchase and more like an ongoing commitment to safety. Keeping your program in top shape involves a few key practices that protect your investment, your people, and your organization. By focusing on routine maintenance, clear protocols, and a prepared team, you can build a program that remains reliable and compliant for years to come.
Set Up Regular Inspections and Reminders
An AED can’t help anyone if its battery is dead or its electrode pads have expired. That’s why regular, hands-on inspections are non-negotiable. The best way to ensure this happens is to assign a specific person or team to be responsible for checking each device. These inspections should follow a consistent schedule—typically monthly—and include verifying the AED’s status indicator, checking the expiration dates on batteries and pads, and making sure rescue kit supplies are fully stocked. A simple checklist and calendar reminders can make all the difference in catching issues before they become critical failures during an emergency.
Use Remote Monitoring to Track Readiness
For organizations with more than one AED, especially across multiple sites, manual inspections can become a logistical headache. This is where technology can be a huge help. Remote monitoring systems automatically track the readiness of every AED in your program, 24/7. These systems can send you real-time alerts if a battery is low, a pad is nearing expiration, or if a device fails its self-test. This automated oversight provides incredible peace of mind and helps you manage your entire fleet of devices efficiently, ensuring every single one is ready for use without the burden of constant manual checks.
Establish Clear Post-Event Protocols
It’s easy to focus on what happens before and during a cardiac arrest event, but what happens after is just as important for your program’s long-term health. If an AED is used, you need a clear, step-by-step plan. This protocol should outline how to secure the device, preserve its event data for medical review, and get it restocked and back in service as quickly as possible. A comprehensive AED program management partner will handle this entire process for you, often providing a loaner AED so your facility is never left unprotected while the original unit is being serviced.
Build a Culture of Preparedness
The most well-maintained AED in the world won’t do any good if your team doesn’t know where it is or what to do. True preparedness goes beyond the device itself; it’s about your people. You can build a strong culture of preparedness by making sure everyone in your organization knows the location of your AEDs and understands the emergency response plan. Use clear signage to point the way to each device. Regularly communicate about the program in newsletters or team meetings. When your entire team feels confident and aware, you create an environment where people are empowered to act decisively when seconds matter most.
Nailing Your Compliance and Documentation
Having an AED is the first step, but proving your program is effective and compliant is just as critical. Solid documentation isn’t just about checking boxes; it’s about creating a clear, defensible record that shows you’ve done everything right. From following federal guidelines to keeping meticulous maintenance logs, getting your paperwork in order protects your organization and ensures your program is always ready for action—and for any audit that might come your way.
Following OSHA and State Rules
Think of your AED program as having two sets of rules to follow: federal and state. At the federal level, OSHA provides guidance for worksite AED programs, emphasizing the need for things like physician oversight and coordination with local emergency services. But the rules don’t stop there. Each state has its own specific requirements for AEDs, which can cover everything from placement to training. Keeping up with both can feel like a full-time job, but it’s a non-negotiable part of responsible AED ownership. A well-managed program ensures you meet every requirement, keeping your people safe and your organization protected.
Registering Your AEDs with Local EMS
One of the most important—and often missed—compliance steps is registering your device with local Emergency Medical Services (EMS). Why does this matter? When someone calls 911, the dispatcher can see a registered AED nearby and direct the caller to it, potentially saving precious minutes. Most states actually require you to coordinate your AED program with local first responders. This registration process, along with providing data after an AED is used, is typically handled by your program’s medical director or coordinator. It’s a simple step that connects your device to the larger community emergency response system, making it even more effective.
Keeping Your Records Audit-Ready
If an incident occurs, your records will be your program’s best defense. That’s why keeping everything audit-ready is so important. This means having organized, easily accessible documentation for every aspect of your program: monthly inspection logs, battery and pad expiration dates, team training certifications, and post-event reports. Manually tracking this on a spreadsheet is a recipe for errors and gaps. Modern AED program management software automates these tasks, sending reminders and creating a digital paper trail. This ensures that if you ever need to demonstrate compliance, you have a complete, accurate history at your fingertips, giving you total confidence in your program.
Related Articles
- Medical Direction and Oversight: What It Is and Why It Matters
- AED Program Management | Compliance and Maintenance
Frequently Asked Questions
I have an AED at my facility. Isn’t that enough? Having an AED is a great start, but the device itself is only one piece of the puzzle. A successful program ensures the AED is always ready to work, your team is prepared to use it, and your organization is compliant with state laws. Without active management, it’s incredibly easy for batteries to die or pads to expire unnoticed, which means the device could fail when you need it most. Program management closes these gaps to make sure your good intentions translate into real readiness.
Do I really need a doctor to oversee my AED program? Yes, in most cases, you do. This is called medical direction, and it’s a legal requirement in many states. A physician provides the necessary prescription to own an AED and ensures your emergency plan follows clinical best practices. This oversight is also one of your strongest protections against liability, as it demonstrates you’ve taken the proper steps to create a safe and effective program.
What’s the most common reason an AED program fails? The single biggest point of failure is a lack of readiness due to expired supplies. The batteries and electrode pads in an AED have a limited shelf life, and if they aren’t replaced on time, the device simply won’t work. Many organizations without a formal management system lose track of these dates, only discovering the problem during an actual emergency when it’s tragically too late.
Can I manage my own AED program, or do I need to hire a service? While you can certainly manage your own program, it requires a significant commitment. You would be responsible for tracking all expiration dates, performing and logging monthly inspections, staying current on changing state regulations, and securing your own physician for medical oversight. A program management partner handles all of these details for you, which saves time and reduces the risk of critical tasks falling through the cracks.
What does AED program management typically cost? The cost is usually structured as an annual fee per device, often starting around $150. It’s best to think of this not as a cost, but as an investment in compliance, liability protection, and peace of mind. This fee covers the expert oversight and automated systems that ensure your AED is ready to save a life, which protects your organization from the far greater costs of a program that isn’t properly maintained.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• ResponseReady.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.