One of the biggest risks for any organization with an AED program is falling out of compliance without even realizing it. Many business owners believe that simply having a device is enough, but the reality is far more detailed. Each state has its own laws governing everything from how often you must inspect your device to whether it needs to be registered with local emergency services. Failing to keep up with these specific AED requirements by state can expose your organization to significant liability and fines. This article will clear up the confusion, breaking down what you need to do to ensure your program is fully compliant and audit-ready.
Key Takeaways
- Compliance is local, not federal: Your AED program must follow the specific laws of your state, which dictate everything from required training and maintenance schedules to device registration with local EMS.
- Readiness depends on consistent upkeep: An effective AED program goes beyond just owning the device; it requires regular inspections, diligent tracking of expiration dates for pads and batteries, and ongoing team training.
- A management system is your best defense: To avoid liability and ensure every device is prepared, implement a documented compliance plan or use a professional service to manage inspections, track requirements, and keep your program audit-ready.
How Do AED Laws Work in the U.S.?
If you’re managing AEDs for your organization, you’ve likely discovered that the rules can feel like a moving target. There isn’t one single set of regulations that applies everywhere in the country. Instead, AED compliance is governed by a mix of federal guidelines and specific state laws, which creates a complex legal landscape. Understanding how these two layers of regulation work together is the first step toward building a compliant and effective AED program that keeps your people safe and your organization protected.
Federal vs. State Regulations
At the federal level, agencies like the Food and Drug Administration (FDA) regulate the manufacturing and sale of AED devices themselves to ensure they are safe and effective. The Occupational Safety and Health Administration (OSHA) also provides guidance on having AEDs in the workplace as part of a first-aid program. However, these federal rules are just the starting point. The day-to-day requirements for owning and maintaining an AED are almost always determined by state-specific laws. Think of federal regulations as the foundation, while state laws build the rest of the house, dictating everything from placement and training to maintenance and registration.
Why Requirements Vary by State
Each state has the authority to create its own laws around AEDs, and they vary quite a bit. What’s required in California might be completely different from the rules in Texas or New York. These differences exist because each state legislature sets its own public health priorities. For example, one state might pass a law requiring AEDs in all schools after a local incident, while another might focus on placing them in gyms or large office buildings. These varying requirements cover who needs CPR and AED training, how often devices must be inspected, and whether you need to register your AED with local emergency services. For businesses operating in multiple states, this creates a significant compliance challenge, making expert program management essential.
Where Are AEDs Required in Public Spaces?
AED requirements aren’t one-size-fits-all. The laws depend entirely on your state and the type of facility you manage. Generally, regulations focus on places where large groups of people gather, learn, or exercise, since these are areas where a sudden cardiac arrest is more likely to occur or be witnessed. Understanding where your organization fits into these categories is the first step toward ensuring you’re compliant and prepared. Below, we’ll walk through the common requirements for different types of public spaces.
Schools and Universities
Protecting students and staff is a top priority, which is why schools are one of the most frequently regulated environments for AEDs. Currently, 25 states mandate that schools have AEDs on-site. These laws often specify that devices must be accessible in high-traffic areas like gymnasiums or near athletic fields, where the risk of cardiac arrest can be higher. Beyond just having the device, many states also focus on preparedness. About 30 states encourage or require students to receive AED and CPR training before graduation. A well-managed AED program ensures your campus is not only equipped but also ready to respond effectively.
Gyms and Fitness Centers
Given the strenuous activity that happens at gyms, it’s no surprise they are often required to have AEDs. At least 13 states have laws mandating AEDs in health clubs and fitness centers. However, the specifics can vary quite a bit. Some laws only apply to facilities over a certain square footage or with a minimum number of members. As a gym owner or manager, it’s critical to check your state and local statutes to see what applies to you. For many facilities, an AED rental program can be a flexible and cost-effective way to meet legal requirements while protecting your members.
Offices and Workplaces
While there are no federal laws that require AEDs in every office, every state has its own set of regulations that may apply. For most private businesses, implementing an AED program is considered a best practice rather than a strict legal mandate. However, choosing to place an AED in your workplace often comes with other responsibilities, such as routine maintenance, staff training, and medical oversight. Establishing a clear and compliant program not only protects your employees but also helps reduce your organization’s liability. A comprehensive management service can handle these details for you, giving you peace of mind.
Government and Public Buildings
Government and public buildings are among the most consistently regulated locations for AEDs. All 50 states have laws or administrative rules that address having AEDs in public spaces like courthouses, airports, community centers, and other municipal facilities. The reasoning is simple: these are high-traffic areas where thousands of people pass through daily, increasing the statistical likelihood of a cardiac emergency. By placing AEDs in these visible and accessible locations, communities can significantly shorten the response time for sudden cardiac arrest. As experts in public access defibrillation, our team helps public sector organizations manage compliant, life-saving programs.
What Training Is Required to Use an AED?
While modern AEDs are designed with simple, step-by-step instructions for almost anyone to use, proper training is a critical piece of any successful emergency response plan. Not only does it build the confidence needed to act decisively during a crisis, but it’s also often a legal requirement. Knowing what kind of training your team needs is the first step toward ensuring your workplace is truly prepared for a sudden cardiac arrest event.
Training Requirements by State
Training mandates are not one-size-fits-all; they vary significantly depending on where your organization is located. Some states require certified training for designated responders in any facility with an AED, while others simply recommend it as a best practice. Because these rules can be so different, many organizations are unknowingly out of compliance with their local AED legislation. It’s essential to check your state and local requirements to confirm your training program is up to code. This ensures your team is prepared and your organization is protected from potential liability.
CPR vs. AED Certification
Effective emergency response training should cover both AED use and cardiopulmonary resuscitation (CPR). The two skills go hand-in-hand. While an AED analyzes the heart’s rhythm and delivers a shock when needed, CPR keeps oxygenated blood flowing to the brain and other vital organs. Most nationally recognized programs, like those offered by the American Heart Association, combine these skills into a single certification course. This integrated approach prepares responders to handle the entire sequence of care for a sudden cardiac arrest victim, from calling 911 to performing chest compressions and using the AED.
Recertification and Ongoing Training
CPR and AED certifications typically expire every two years, so ongoing training is essential for maintaining readiness and compliance. Regular refresher courses ensure your team’s skills stay sharp and that they remember what to do when every second counts. More importantly, consistent training builds confidence, which is crucial for overcoming the hesitation to act in a real emergency. A comprehensive AED management program can help you track certification deadlines for your entire team, making it easy to schedule recertification courses and ensure your responders are always prepared. This commitment to ongoing education strengthens your workplace safety culture and can dramatically improve outcomes.
How Do Good Samaritan Laws Protect AED Users?
One of the biggest hesitations people have about using an AED is the fear of doing something wrong. What if you hurt the person? What if you get sued? Thankfully, every state has laws in place to protect people who step up to help in an emergency. These laws are designed to give you the confidence to act when someone’s life is on the line. Let’s clear up how they work and address some common fears.
Understanding Liability Protection
If you’ve ever worried about the legal risks of using an AED, you can breathe a little easier. Good Samaritan laws exist in all 50 states to protect bystanders who act in good faith during an emergency. In simple terms, these laws shield you from liability if you use an AED to help someone experiencing sudden cardiac arrest. The goal is to encourage people to act quickly without fearing a lawsuit. This protection applies as long as you aren’t grossly negligent or intentionally causing harm, which is a very high bar to meet. As long as you are genuinely trying to help, the law is on your side.
Common Myths About Using an AED
The fear of legal trouble fuels a lot of myths about using an AED. Many people believe they need extensive medical training or that they could accidentally harm the person. The truth is, modern AEDs are designed for anyone to use, providing clear, step-by-step voice instructions. They won’t deliver a shock unless a life-threatening heart rhythm is detected, making them incredibly safe. While these laws protect the rescuer, it’s important to remember that the organization that owns the device is still responsible for its upkeep. Failing to meet your state’s AED compliance requirements for maintenance and readiness can create serious liability risks for your business.
What Are the State Requirements for AED Maintenance?
An AED is only effective if it’s ready to work at a moment’s notice. That’s why state laws don’t just cover where to place an AED; they also outline specific maintenance requirements to ensure every device is functional and compliant. Simply mounting an AED on the wall and hoping for the best isn’t enough to protect your organization or the people you serve. These rules are in place to make sure your device is always prepared for an emergency. Let’s look at the three core components of AED maintenance that most states require.
Daily, Monthly, and Annual Inspections
Regular inspections are the foundation of a reliable AED program. Most states mandate routine checks to confirm your AED is accessible, visible, and ready for use. These inspections often involve verifying the green readiness light is flashing and checking that supplies are intact. The required frequency can vary, with some locations needing quick daily checks while others follow a monthly schedule. Managing these inspections across multiple sites can become a serious challenge, especially when different state laws apply. A consistent AED program management plan is key to staying on top of every device without letting anything fall through the cracks.
Documentation and Record-Keeping
If you can’t prove it, it didn’t happen. That’s why meticulous record-keeping is a non-negotiable part of AED compliance. After every inspection, you need to document the date, the inspector’s name, and the device’s status. This log serves as your official record that you are meeting state requirements and manufacturer guidelines. In the event of an incident or an audit, this documentation is your proof of due diligence and is essential for liability protection. Keeping organized records for every AED shows your program is fully compliant and ready for scrutiny.
Battery and Pad Replacement Schedules
An AED’s battery and electrode pads are its most critical components, and both have expiration dates. A dead battery or dried-out pads can render the device useless. State laws require organizations to follow the manufacturer’s recommended replacement schedule to keep AEDs operational. Forgetting to replace these parts is a common compliance failure. Tracking expiration dates for a single device is manageable, but the task becomes complex with multiple AEDs. Staying ahead of these deadlines by ordering and installing new AED accessories before they expire is vital for ensuring your device will function when it matters most.
What Are the Rules for AED Registration and Oversight?
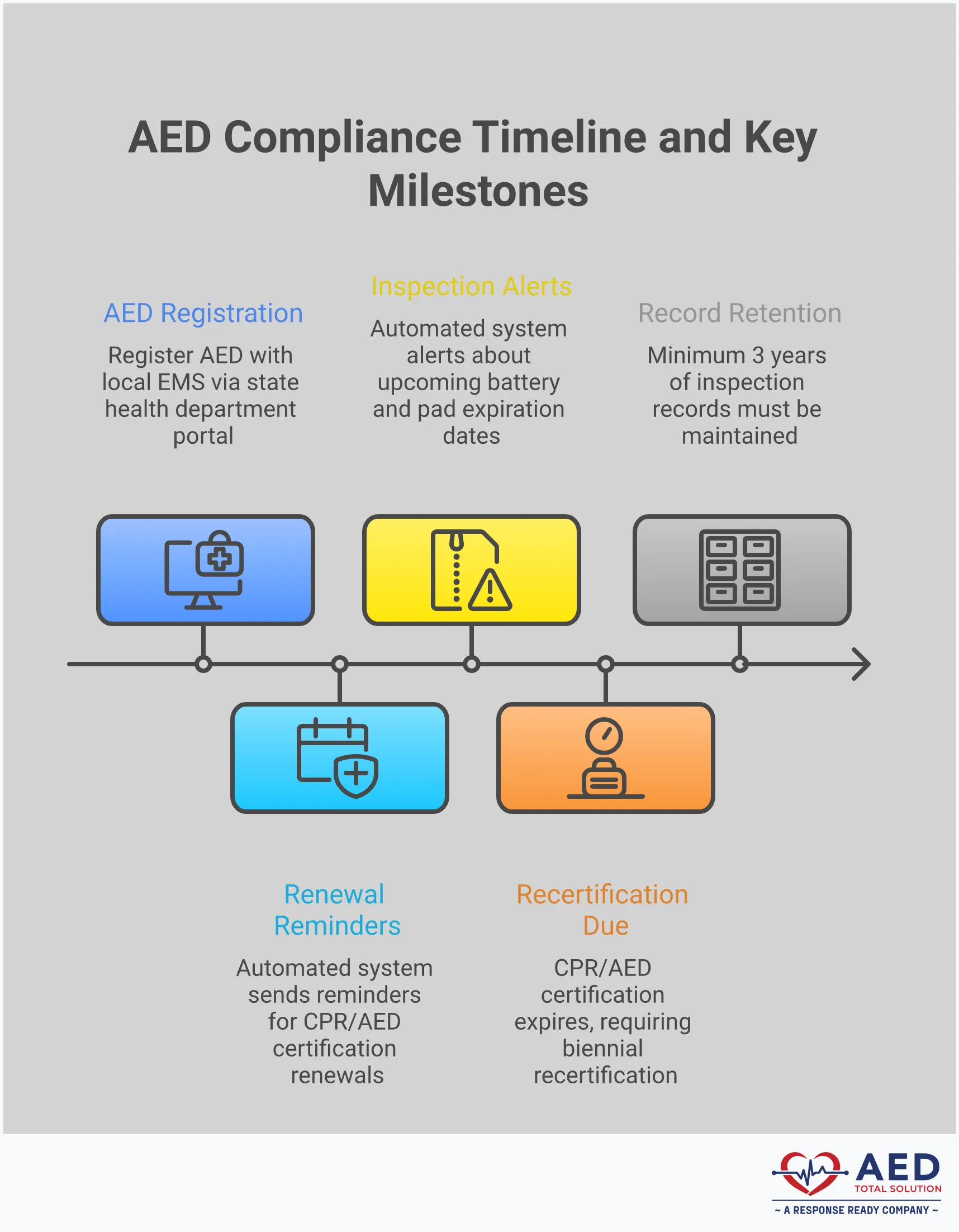
Beyond simply placing an AED on the wall, a truly effective program involves clear rules for registration and oversight. These requirements aren’t just about checking boxes; they are designed to ensure your device is properly managed and integrated into the local emergency response system. When an AED is registered, 911 dispatchers can direct callers to its location, potentially saving precious minutes during a cardiac arrest. Proper oversight, which includes everything from routine inspections to tracking expiration dates, ensures the device is always ready to perform as expected.
Unfortunately, many organizations are unaware of their state’s specific AED requirements, which leaves them vulnerable to compliance gaps and potential liability. The rules can feel complicated because they often involve multiple layers of regulations from state and local agencies. For example, some jurisdictions require you to notify local EMS after each use, while others have specific documentation standards you must follow. Understanding these key components of AED program management is the first step toward building a reliable and compliant safety net for your employees, customers, and visitors. A well-managed program gives you confidence that your AED will be an asset, not a liability, when it’s needed most.
Which States Require AED Registration?
Many states require you to register your AED with local emergency medical services (EMS) or another designated agency. The primary reason for this is to add your device to a community-wide database. When someone calls 911 to report a cardiac arrest, the dispatcher can see your AED on their map and tell the caller where to find it. This simple step can turn a bystander into a first responder.
Because AED legislation varies so much from one state to another, it’s critical to know your local rules. Some states have strict mandates for registration and reporting, while others simply recommend it as a best practice. Failing to register your device where required can not only result in penalties but also means your community loses a life-saving resource.
The Role of a Medical Director
In many states, an AED program must be overseen by a medical director, who is a licensed physician responsible for ensuring the program follows established medical protocols. This individual provides medical oversight, which can include writing and approving the emergency response plan, reviewing AED usage data after an event, and ensuring that the program aligns with state and local laws.
Think of the medical director as the clinical authority for your program. Their involvement ensures your procedures are sound and that your team is prepared to respond correctly. Having a physician oversee your program is often a key requirement for qualifying for Good Samaritan law protection. Our program management services include access to medical oversight to help you meet these important compliance standards.
Coordinating with Emergency Services
Registering your AED is the first step, but ongoing coordination with emergency services is what makes your program truly effective. This means ensuring your local 911 dispatch center has accurate, up-to-date information about your device’s location, accessibility, and readiness status. If you move the AED to a different floor or your building’s access hours change, that information needs to be communicated.
For organizations with devices across multiple sites, this coordination becomes even more complex. You could be dealing with dozens of different EMS agencies, each with its own procedures. Strong communication ensures a seamless handoff between your internal responders and the professional crews who arrive on the scene. This is a core part of a comprehensive AED program that keeps your entire system connected and ready.
What Are the Most Common AED Compliance Myths?
When it comes to AED compliance, misinformation can be just as dangerous as a dead battery. Believing a common myth can leave your organization exposed to liability and your AED unprepared for an emergency. Let’s clear up a few of the most persistent misconceptions so you can feel confident that your program is protected, documented, and ready when seconds matter most. Understanding these truths is the first step toward building an effective and compliant AED program.
Myth: Federal Guidelines Are Enough
Many people assume following federal guidelines covers all their bases. While federal laws like the Cardiac Arrest Survival Act offer a foundation by providing Good Samaritan protections, they are only part of the story. The reality is that AED regulation is handled at the state level. Each state has its own set of specific requirements dictating everything from where an AED must be placed to who needs to be notified of its location. Relying solely on federal guidance is a common mistake that can result in non-compliance and create significant legal risks for your organization.
Myth: Underestimating Training and Maintenance
Placing an AED on the wall is a great first step, but it’s not the last one. The belief that the device alone ensures readiness overlooks two critical components: proper training and consistent maintenance. An AED is only effective if someone knows how to use it confidently in an emergency, and many states require CPR and AED training for responders. Just as important, the device must be functional. Regular inspections, battery replacements, and pad expirations are often legal requirements, not just best practices. A comprehensive program management service ensures these details are never missed.
Myth: Overlooking Multi-State Challenges
If you manage AEDs in more than one state, it’s easy to think a single compliance strategy will work everywhere. This approach can quickly lead to problems. Managing devices across multiple sites is complex, and that complexity grows with each state line you cross. What satisfies compliance in California may not meet the requirements in Texas or New York. Each state has different rules for registration, medical oversight, and maintenance documentation. This creates a patchwork of regulations that is difficult to track, especially for multi-location organizations. A one-size-fits-all approach simply doesn’t work.
How Can You Stay Compliant with State AED Laws?
Keeping up with different state AED laws can feel like a full-time job, but it doesn’t have to be. With a clear strategy, you can build a program that protects your organization and ensures your devices are always ready for an emergency. A proactive approach to compliance isn’t just about following rules; it’s about creating a safe environment where everyone feels prepared. Here’s how you can get started.
Create a Comprehensive Compliance Program
Navigating AED requirements by state may seem daunting, but a structured plan makes all the difference. A solid compliance program should cover every part of your AED’s lifecycle, from initial placement and registration to ongoing maintenance and staff training. Document everything: inspection dates, battery and pad expiration dates, and training certifications. This creates a clear, auditable record that proves your commitment to readiness. Ensuring your devices are accessible, functional, and compliant is the core goal, and a well-documented program is your roadmap to achieving it. A complete approach removes the guesswork and gives you confidence in your emergency response plan.
Track Inspections Across All Locations
Managing one AED has its challenges, but overseeing devices across multiple sites adds another layer of complexity. Each location might fall under different local or state rules, and you need a system to confirm every device is inspected on schedule. Relying on manual spreadsheets or email reminders often leads to missed checks and compliance gaps. A centralized tracking system is essential for multi-location organizations. It gives you a single view of your entire AED inventory, automates reminders, and provides a clear record of all maintenance activities. This way, you can be sure every device, no matter where it is, is properly maintained and ready to use.
Use a Professional AED Management Service
If building and running a compliance program feels overwhelming, you’re not alone. Many organizations choose to partner with a professional service to handle the details. An expert team can simplify AED compliance by managing maintenance schedules, tracking expiration dates, and staying current on changing state laws for you. This approach is especially helpful for businesses without a dedicated safety manager. With full-service AED program management, you get peace of mind knowing every critical task is handled correctly and on time. It’s a straightforward way to protect your organization while ensuring your AEDs are always prepared for an emergency.
What Resources Help You Track State Requirements?
Keeping up with AED laws can feel like a moving target, especially if you manage devices in more than one state. The good news is you don’t have to figure it all out on your own. Several reliable resources can help you find the information you need to keep your program compliant, your team prepared, and your workplace safe. By knowing where to look, you can get clear, accurate answers and build a compliance strategy that works.
State Health Department Websites
Your first stop for official information should always be your state’s health department website. These sites are the primary source for local AED laws, so you can trust that the details are accurate and current. Many organizations are unaware of their state’s specific AED requirements, which can leave them open to penalties. You can find specific rules on everything from device placement and registration to required training and maintenance schedules. It’s a good idea to find your state’s page and bookmark it for future reference. The CDC offers a directory to help you find your local health department’s website.
Professional Compliance Management Tools
If you’re tracking more than one AED, especially across different locations, manual spreadsheets can quickly become a headache. This is where professional compliance management tools can make a huge difference. These systems automate the tracking process, sending you reminders for monthly inspections, battery and pad expirations, and recertification deadlines. Instead of juggling dates and documents, you get a clear, centralized view of your entire program’s readiness. A full-service AED program management partner can handle these details for you, ensuring every device is accounted for and audit-ready. This approach saves time and gives you confidence that nothing will fall through the cracks.
Training and Certification Programs
Training is a cornerstone of any successful AED program, and certification bodies are excellent resources for compliance information. Organizations like the American Red Cross and the American Heart Association don’t just teach you how to use an AED; their instructors are often knowledgeable about state-specific training mandates. Engaging in a formal training and certification program ensures your team meets legal requirements and feels prepared to respond confidently in an emergency. These courses cover the essential skills for both AED use and CPR, which are often required together, making sure your staff is ready to act when it matters most.
What Happens if You’re Not Compliant?
Staying on top of AED requirements isn’t just about checking a box; it’s about protecting your organization and the people you serve. When compliance slips, the consequences can be serious, extending far beyond the immediate emergency. From legal trouble to insurance headaches, failing to maintain your AED program can create significant problems for your business. Let’s look at what’s at stake.
Legal Penalties and Liability Risks
Failing to follow your state’s AED laws can open your organization up to serious legal trouble. Many businesses are simply unaware of their specific obligations, leaving them vulnerable to fines and other penalties. More importantly, if a sudden cardiac arrest occurs and your AED isn’t properly maintained or accessible, you could face civil lawsuits. Adhering to state-specific regulations isn’t optional; it’s a critical step in protecting your organization from increased liability. A well-managed program demonstrates due diligence and a commitment to safety, which is your best defense in a worst-case scenario.
Insurance and Risk Management Issues
Beyond direct legal penalties, non-compliance creates major risk management headaches. Insurance carriers expect organizations to follow all applicable laws, and a compliance failure could complicate a claim or even impact your coverage. Managing an AED program effectively is a key part of your overall safety and risk mitigation strategy. Things like staff turnover can make it easy for tasks to fall through the cracks, but the liability remains. A proactive approach to AED program management ensures your devices are always ready and helps you demonstrate that you’ve taken reasonable steps to protect your employees and visitors, strengthening your position with insurers.
Related Articles
- AED Laws & Requirements Across State — AED Total Solution
- AED Signage Requirements & Laws for Compliance | AED Total Solution
- AED Rules and Regulations: A Compliance Guide
- AED Legal Requirements for Businesses: Stay Compliant
Frequently Asked Questions
Why can’t I just follow one set of rules for all my AEDs? It would certainly be easier if there were a single national standard, but AED compliance is managed at the state level. While federal agencies regulate the devices themselves, each state creates its own laws for ownership, including requirements for placement, training, registration, and maintenance. This means the rules in one state can be completely different from another, making a one-size-fits-all approach a common but risky mistake.
What’s the most common reason an AED program fails? The most frequent point of failure isn’t the device itself, but the lack of consistent oversight. Many well-intentioned programs start strong but fall apart over time when routine tasks are forgotten. This often looks like missed monthly inspections, expired batteries or pads that go unnoticed, or lapsed training certifications for staff. These seemingly small details are what ensure an AED is ready to work during an emergency.
Am I protected from a lawsuit if I use an AED to help someone? Yes, every state has Good Samaritan laws designed to protect bystanders who act in good faith to help during an emergency. These laws shield you from liability as long as you are genuinely trying to save a life and not acting recklessly. The goal is to encourage people to step in and help without the fear of legal consequences.
Do I need a doctor to be involved with my AED program? In many states, yes. This requirement is known as medical oversight, and it means a licensed physician must oversee your program to ensure it follows proper medical protocols. This doctor is responsible for things like approving your response plan and reviewing data after the AED is used. This oversight is often a key condition for qualifying for Good Samaritan law protection.
My business operates in several states. What’s the best way to manage compliance? Managing AEDs across multiple states is a significant challenge because you have to track a different set of rules for each location. The most effective way to handle this is with a centralized management system that can track each state’s specific requirements for inspections, registration, and training. Partnering with a professional management service can remove this burden entirely, ensuring every device in your portfolio is compliant, no matter where it is.
Disclaimer for information purposes only:
The information provided on this website is intended for general educational and informational purposes only. It is not medical advice and should not be used as a substitute for professional diagnosis, treatment, or care. Always consult a qualified healthcare or medical professional regarding any health-related questions or concerns.
While we strive to ensure the information shared is accurate and up to date, no guarantees are made regarding completeness, accuracy, or applicability to any individual situation. Use of this content is at the reader’s sole discretion and risk.
This website is part of the Response Ready family of emergency preparedness and training resources, including CPR & first aid training and compliance services, AED sales and program support, AED program management software, and medical oversight solutions provided through our affiliated platforms:
• CPR1.com
• AEDLeader.com
• ResponseReady.com
• MDSIMedical.com
By accessing or using this website, you agree to release, indemnify, and hold harmless the website owners, authors, contributors, and affiliated entities from any claims, losses, damages, or liabilities arising from the use or reliance on the information presented.